Recurrence Risk after First Symptomatic Distal versus Proximal Deep Vein Thrombosis According to Baseline Risk Factors
- PMID: 31249983
- PMCID: PMC6524909
- DOI: 10.1055/s-0039-1683374
Recurrence Risk after First Symptomatic Distal versus Proximal Deep Vein Thrombosis According to Baseline Risk Factors
Abstract
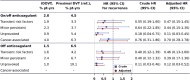
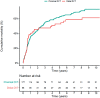
Background It remains unclear whether the distal location of deep vein thrombosis (DVT) is independently associated with a lower risk of recurrence in all patients, or represents a marker of the presence and severity of provoking factors for venous thromboembolism (VTE). Methods We investigated the impact of distal (vs. proximal) DVT location on the risk of developing symptomatic, objectively confirmed recurrent VTE in 831 patients with a first acute symptomatic DVT not associated with pulmonary embolism (PE), who were stratified by the presence of transient or persistent risk factors at baseline. The primary outcome was symptomatic, objectively diagnosed recurrent VTE, including proximal DVT and PE. Results A total of 205 (24.7%) patients presented with a transient risk factor, 189 (22.7%) with a minor persistent risk factor, 202 (24.3%) with unprovoked DVT, and 235 (28.3%) with cancer-associated DVT. One-hundred twenty-five patients (15.0%) experienced recurrent DVT or PE. The largest relative difference between patients with distal (vs. proximal) DVT was observed in the absence of identifiable risk factors (adjusted hazard ratio [aHR]: 0.11; 95% CI [confidence interval]: 0.03-0.45). In patients with cancer, distal and proximal DVT had a comparable risk of recurrence (aHR: 0.70; 95% CI: 0.28-1.78]). Conclusions The distal (vs. proximal) location of first acute symptomatic DVT represented, in the absence of any identifiable transient or persistent risk factors, a favorable prognostic factor for recurrence. In contrast, the prognostic impact of DVT location was weaker if persistent provoking risk factors for VTE were present, notably cancer.
Keywords: epidemiology; prognosis; pulmonary embolism; venous thromboembolism.
Conflict of interest statement
Figures

References
-
- Posch F, Riedl J, Reitter E M et al.Hypercoagulabilty, venous thromboembolism, and death in patients with cancer. A multi-state model. Thromb Haemost. 2016;115(04):817–826. - PubMed
-
- Børvik T, Brækkan S K, Enga K et al.COPD and risk of venous thromboembolism and mortality in a general population. Eur Respir J. 2016;47(02):473–481. - PubMed
-
- Konstantinides S V, Barco S, Lankeit M, Meyer G. Management of pulmonary embolism: an update. J Am Coll Cardiol. 2016;67(08):976–990. - PubMed
-
- Vaitkus P T, Leizorovicz A, Cohen A T, Turpie A G, Olsson C G, Goldhaber S Z; PREVENT Medical Thromboprophylaxis Study Group.Mortality rates and risk factors for asymptomatic deep vein thrombosis in medical patients Thromb Haemost 2005930176–79. - PubMed
-
- Kearon C, Akl E A, Ornelas J et al.Antithrombotic therapy for VTE disease: CHEST Guideline and Expert Panel Report. Chest. 2016;149(02):315–352. - PubMed
LinkOut - more resources
Full Text Sources

