Cost-per-diagnosis as a metric for monitoring cost-effectiveness of HIV testing programmes in low-income settings in southern Africa: health economic and modelling analysis
- PMID: 31287620
- PMCID: PMC6615491
- DOI: 10.1002/jia2.25325
Cost-per-diagnosis as a metric for monitoring cost-effectiveness of HIV testing programmes in low-income settings in southern Africa: health economic and modelling analysis
Abstract
Introduction: As prevalence of undiagnosed HIV declines, it is unclear whether testing programmes will be cost-effective. To guide their HIV testing programmes, countries require appropriate metrics that can be measured. The cost-per-diagnosis is potentially a useful metric.
Methods: We simulated a series of setting-scenarios for adult HIV epidemics and ART programmes typical of settings in southern Africa using an individual-based model and projected forward from 2018 under two policies: (i) a minimum package of "core" testing (i.e. testing in pregnant women, for diagnosis of symptoms, in sex workers, and in men coming forward for circumcision) is conducted, and (ii) core-testing as above plus additional testing beyond this ("additional-testing"), for which we specify different rates of testing and various degrees to which those with HIV are more likely to test than those without HIV. We also considered a plausible range of unit test costs. The aim was to assess the relationship between cost-per-diagnosis and the incremental cost-effectiveness ratio (ICER) of the additional-testing policy. The discount rate used in the base case was 3% per annum (costs in 2018 U.S. dollars).
Results: There was a strong graded relationship between the cost-per-diagnosis and the ICER. Overall, the ICER was below $500 per-DALY-averted (the cost-effectiveness threshold used in primary analysis) so long as the cost-per-diagnosis was below $315. This threshold cost-per-diagnosis was similar according to epidemic and programmatic features including the prevalence of undiagnosed HIV, the HIV incidence and a measure of HIV programme quality (the proportion of HIV diagnosed people having a viral load <1000 copies/mL). However, restricting to women, additional-testing did not appear cost-effective even at a cost-per-diagnosis of below $50, while restricting to men additional-testing was cost-effective up to a cost-per-diagnosis of $585. The threshold cost per diagnosis for testing in men to be cost-effective fell to $256 when the cost-effectiveness threshold was $300 instead of $500, and to $81 when considering a discount rate of 10% per annum.
Conclusions: For testing programmes in low-income settings in southern African there is an extremely strong relationship between the cost-per-diagnosis and the cost-per-DALY averted, indicating that the cost-per-diagnosis can be used to monitor the cost-effectiveness of testing programmes.
Keywords: HIV; cost-effectiveness; health systems; modelling; testing.
© 2019 The Authors. Journal of the International AIDS Society published by John Wiley & Sons Ltd on behalf of the International AIDS Society.
Figures

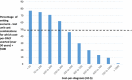

References
-
- De Cock KM, Barker JL, Baggaley R, El Sadr WM. Where are the positives? HIV testing in sub‐Saharan Africa in the era of test and treat. AIDS. 2019;33:349–52. - PubMed
-
- UNAIDS . 90‐90‐90 An ambitious treatment target to help end the AIDS epidemic. 2014. [cited 2019 May 31]. Available from: http://www.unaids.org/sites/default/files/media_asset/90-90-90_en_0.pdf
-
- UNAIDS . Fast‐track update on investments needed in the AIDS response. 2016. [cited 2019 May 31]. Available from: http://www.unaids.org/en/resources/documents/2014/JC2686_WAD2014report
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

