Factors associated with poor adherence to medication among hypertensive patients in twelve low and middle income Sub-Saharan countries
- PMID: 31291293
- PMCID: PMC6619761
- DOI: 10.1371/journal.pone.0219266
Factors associated with poor adherence to medication among hypertensive patients in twelve low and middle income Sub-Saharan countries
Abstract
Introduction: Over the past few decades, the prevalence of hypertension has dramatically increased in Sub-Saharan Africa. Poor adherence has been identified as a major cause of failure to control hypertension. Scarce data are available in Africa.
Aims: We assessed adherence to medication and identified socioeconomics, clinical and treatment factors associated with low adherence among hypertensive patients in 12 sub-Saharan African countries.
Method: We conducted a cross-sectional survey in urban clinics of both low and middle income countries. Data were collected by physicians on demographics, treatment and clinical data among hypertensive patients attending the clinics. Adherence was assessed by questionnaires completed by the patients. Factors associated with low adherence were investigated using logistic regression with a random effect on countries.
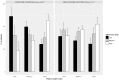
Results: There were 2198 individuals from 12 countries enrolled in the study. Overall, 678 (30.8%), 738 (33.6%), 782 (35.6%) participants had respectively low, medium and high adherence to antihypertensive medication. Multivariate analysis showed that the use of traditional medicine (OR: 2.28, 95%CI [1.79-2.90]) and individual wealth index (low vs. high wealth: OR: 1.86, 95%CI [1.35-2.56] and middle vs. high wealth: OR: 1.42, 95%CI [1.11-1.81]) were significantly and independently associated with poor adherence to medication. In stratified analysis, these differences in adherence to medication according to individual wealth index were observed in low-income countries (p<0.001) but not in middle-income countries (p = 0.17). In addition, 26.5% of the patients admitted having stopped their treatment due to financial reasons and this proportion was 4 fold higher in the lowest than highest wealth group (47.8% vs 11.4%) (p<0.001).
Conclusion: This study revealed the high frequency of poor adherence in African patients and the associated factors. These findings should be useful for tailoring future programs to tackle hypertension in low income countries that are better adapted to patients, with a potential associated enhancement of their effectiveness.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures



Similar articles
-
Socioeconomic Status and Hypertension Control in Sub-Saharan Africa: The Multination EIGHT Study (Evaluation of Hypertension in Sub-Saharan Africa).Hypertension. 2018 Apr;71(4):577-584. doi: 10.1161/HYPERTENSIONAHA.117.10512. Epub 2018 Jan 29. Hypertension. 2018. PMID: 29378852
-
Poor adherence to medication and salt restriction as a barrier to reaching blood pressure control in patients with hypertension: Cross-sectional study from 12 sub-Saharan countries.Arch Cardiovasc Dis. 2020 Jun-Jul;113(6-7):433-442. doi: 10.1016/j.acvd.2019.11.009. Epub 2020 May 17. Arch Cardiovasc Dis. 2020. PMID: 32434710
-
The state of hypertension care in 44 low-income and middle-income countries: a cross-sectional study of nationally representative individual-level data from 1·1 million adults.Lancet. 2019 Aug 24;394(10199):652-662. doi: 10.1016/S0140-6736(19)30955-9. Epub 2019 Jul 18. Lancet. 2019. PMID: 31327566
-
Reasons for poor blood pressure control in Eastern Sub-Saharan Africa: looking into 4P's (primary care, professional, patient, and public health policy) for improving blood pressure control: a scoping review.BMC Cardiovasc Disord. 2021 Mar 4;21(1):123. doi: 10.1186/s12872-021-01934-6. BMC Cardiovasc Disord. 2021. PMID: 33663387 Free PMC article.
-
Urban-rural differences in hypertension prevalence in low-income and middle-income countries, 1990-2020: A systematic review and meta-analysis.PLoS Med. 2022 Aug 25;19(8):e1004079. doi: 10.1371/journal.pmed.1004079. eCollection 2022 Aug. PLoS Med. 2022. PMID: 36007101 Free PMC article.
Cited by
-
Medication Adherence Interventions for Cardiovascular Disease in Low- and Middle-Income Countries: A Systematic Review.Patient Prefer Adherence. 2021 Apr 29;15:885-897. doi: 10.2147/PPA.S296280. eCollection 2021. Patient Prefer Adherence. 2021. PMID: 33953548 Free PMC article. Review.
-
Worldwide study of the taste of bitter medicines and their modifiers.bioRxiv [Preprint]. 2024 Apr 28:2024.04.24.590957. doi: 10.1101/2024.04.24.590957. bioRxiv. 2024. Update in: Chem Senses. 2025 Jan 22;50:bjaf003. doi: 10.1093/chemse/bjaf003. PMID: 38712219 Free PMC article. Updated. Preprint.
-
Estimating the Lifetime Cost of Managing Hypertension in Ghana: A Modelling Study.Health Serv Insights. 2024 Mar 29;17:11786329241241909. doi: 10.1177/11786329241241909. eCollection 2024. Health Serv Insights. 2024. PMID: 38559500 Free PMC article.
-
Factors affecting adherence to hypertension medications in hypertensive patients attending to primary health care units in Bahrain.J Family Med Prim Care. 2025 Jun;14(6):2336-2345. doi: 10.4103/jfmpc.jfmpc_1116_24. Epub 2025 Jun 30. J Family Med Prim Care. 2025. PMID: 40726715 Free PMC article.
-
Pharmacogenomics of Hypertension in Africa: Paving the Way for a Pharmacogenetic-Based Approach for the Treatment of Hypertension in Africans.Int J Hypertens. 2023 May 30;2023:9919677. doi: 10.1155/2023/9919677. eCollection 2023. Int J Hypertens. 2023. PMID: 38633331 Free PMC article. Review.
References
-
- NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in blood pressure from 1975 to 2015: a pooled analysis of 1479 population-based measurement studies with 19.1 million participants. Lancet (London, England). 2017;389(10064):37–55. Epub 2016/11/20. 10.1016/s0140-6736(16)31919-5 - DOI - PMC - PubMed
-
- Bramley TJ, Gerbino PP, Nightengale BS, Frech-Tamas F. Relationship of blood pressure control to adherence with antihypertensive monotherapy in 13 managed care organizations. Journal of managed care pharmacy: JMCP. 2006;12(3):239–45. Epub 2006/04/21. 10.18553/jmcp.2006.12.3.239 . - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

