Development and validation of a patient decision aid for prostate Cancer therapy: from paternalistic towards participative shared decision making
- PMID: 31296199
- PMCID: PMC6624887
- DOI: 10.1186/s12911-019-0862-4
Development and validation of a patient decision aid for prostate Cancer therapy: from paternalistic towards participative shared decision making
Abstract
Background: Patient decision aids (PDAs) can support the treatment decision making process and empower patients to take a proactive role in their treatment pathway while using a shared decision-making (SDM) approach making participatory medicine possible. The aim of this study was to develop a PDA for prostate cancer that is accurate and user-friendly.
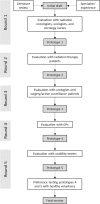
Methods: We followed a user-centered design process consisting of five rounds of semi-structured interviews and usability surveys with topics such as informational/decisional needs of users and requirements for PDAs. Our user-base consisted of 8 urologists, 4 radiation oncologists, 2 oncology nurses, 8 general practitioners, 19 former prostate cancer patients, 4 usability experts and 11 healthy volunteers.
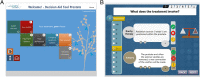
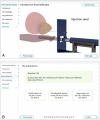
Results: Informational needs for patients centered on three key factors: treatment experience, post-treatment quality of life, and the impact of side effects. Patients and clinicians valued a PDA that presents balanced information on these factors through simple understandable language and visual aids. Usability questionnaires revealed that patients were more satisfied overall with the PDA than clinicians; however, both groups had concerns that the PDA might lengthen consultation times (42 and 41%, respectively). The PDA is accessible on http://beslissamen.nl/ .
Conclusions: User-centered design provided valuable insights into PDA requirements but challenges in integrating diverse perspectives as clinicians focus on clinical outcomes while patients also consider quality of life. Nevertheless, it is crucial to involve a broad base of clinical users in order to better understand the decision-making process and to develop a PDA that is accurate, usable, and acceptable.
Keywords: Patient decision aid; Patient education; Prostate cancer; Shared decision-making; User-centered design.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures





References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

