Inadequate oral feeding as a barrier to discharge in moderately preterm infants
- PMID: 31296918
- PMCID: PMC7246972
- DOI: 10.1038/s41372-019-0422-x
Inadequate oral feeding as a barrier to discharge in moderately preterm infants
Abstract
Objectives: The objectives describe the frequency that inadequate oral feeding (IOF) is the reason why moderately preterm (MPT) infants remain hospitalized and its association with neonatal morbidities.
Study design: Prospective study using the NICHD Neonatal Research Network MPT Registry. Multivariable logistic regression was used to describe associations between IOF and continued hospitalization at 36 weeks postmenstrual age (PMA).
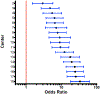
Result: A total of 6017 MPT infants from 18 centers were included. Three-thousand three-seventy-six (56%) remained hospitalized at 36 weeks PMA, of whom 1262 (37%) remained hospitalized due to IOF. IOF was associated with RDS (OR 2.02, 1.66-2.46), PDA (OR 1.86, 1.37-2.52), sepsis (OR 2.36, 95% 1.48-3.78), NEC (OR 16.14, 7.27-35.90), and BPD (OR 3.65, 2.56-5.21) compared to infants discharged and was associated with medical NEC (OR 2.06, 1.19-3.56) and BPD (OR 0.46, 0.34-0.61) compared to infants remaining hospitalized for an alternative reason.
Conclusion: IOF is the most common barrier to discharge in MPT infants, especially among those with neonatal morbidities.
Conflict of interest statement
Figures
References
-
- Eichenwald EC, Blackwell M, Lloyd JS, Tran T, Wilker RE, Richardson DK. Inter-neonatal intensive care unit variation in discharge timing: influence of apnea and feeding management. Pediatrics. 2001;108(4):928–33. - PubMed
-
- Bakewell-Sachs S, Medoff-Cooper B, Escobar GJ, Silber JH, Lorch SA. Infant functional status: the timing of physiologic maturation of premature infants. Pediatrics. 2009;123(5):e878–86. - PubMed
-
- Lau C Oral Feeding in the Preterm Infant. NeoReviews. 2006;7(1):e19–e27.
-
- Mizuno K, Ueda A. Neonatal feeding performance as a predictor of neurodevelopmental outcome at 18 months. Developmental medicine and child neurology. 2005;47(5):299–304. - PubMed
-
- Torola H, Lehtihalmes M, Yliherva A, Olsen P. Feeding skill milestones of preterm infants born with extremely low birth weight (ELBW). Infant behavior & development. 2012;35(2):187–94. - PubMed
Publication types
MeSH terms
Grants and funding
- UG1 HD068263/HD/NICHD NIH HHS/United States
- UL1 TR001111/TR/NCATS NIH HHS/United States
- U10 HD021385/HD/NICHD NIH HHS/United States
- U10 HD021364/HD/NICHD NIH HHS/United States
- UG1 HD068270/HD/NICHD NIH HHS/United States
- UL1 TR000442/TR/NCATS NIH HHS/United States
- UG1 HD027856/HD/NICHD NIH HHS/United States
- UG1 HD034216/HD/NICHD NIH HHS/United States
- UL1 TR000454/TR/NCATS NIH HHS/United States
- UG1 HD027904/HD/NICHD NIH HHS/United States
- UG1 HD040492/HD/NICHD NIH HHS/United States
- M01 RR000080/RR/NCRR NIH HHS/United States
- U24 HD095254/HD/NICHD NIH HHS/United States
- U10 HD027856/HD/NICHD NIH HHS/United States
- U10 HD021373/HD/NICHD NIH HHS/United States
- U10 HD027880/HD/NICHD NIH HHS/United States
- U10 HD053109/HD/NICHD NIH HHS/United States
- UL1 TR000042/TR/NCATS NIH HHS/United States
- UL1 TR000006/TR/NCATS NIH HHS/United States
- UG1 HD040689/HD/NICHD NIH HHS/United States
- UL1 TR001449/TR/NCATS NIH HHS/United States
- UG1 HD053089/HD/NICHD NIH HHS/United States
- UL1 TR002489/TR/NCATS NIH HHS/United States
- UL1 TR000093/TR/NCATS NIH HHS/United States
- U10 HD040689/HD/NICHD NIH HHS/United States
- U10 HD040492/HD/NICHD NIH HHS/United States
- U10 HD027853/HD/NICHD NIH HHS/United States
- U10 HD027904/HD/NICHD NIH HHS/United States
- U10 HD068244/HD/NICHD NIH HHS/United States
- U10 HD068263/HD/NICHD NIH HHS/United States
- U10 HD068270/HD/NICHD NIH HHS/United States
- UL1 TR000041/TR/NCATS NIH HHS/United States
- U10 HD027851/HD/NICHD NIH HHS/United States
- UL1 TR001117/TR/NCATS NIH HHS/United States
- U10 HD068284/HD/NICHD NIH HHS/United States
- UL1 TR000077/TR/NCATS NIH HHS/United States
- UG1 HD053109/HD/NICHD NIH HHS/United States
- U10 HD068278/HD/NICHD NIH HHS/United States
- U10 HD034216/HD/NICHD NIH HHS/United States
- U10 HD036790/HD/NICHD NIH HHS/United States
- U10 HD053089/HD/NICHD NIH HHS/United States
- UL1 TR003142/TR/NCATS NIH HHS/United States