Association of Lifespan Cognitive Reserve Indicator With Dementia Risk in the Presence of Brain Pathologies
- PMID: 31302677
- PMCID: PMC6628596
- DOI: 10.1001/jamaneurol.2019.2455
Association of Lifespan Cognitive Reserve Indicator With Dementia Risk in the Presence of Brain Pathologies
Abstract
Importance: Evidence on the association of lifespan cognitive reserve (CR) with dementia is limited, and the strength of this association in the presence of brain pathologies is unknown.
Objective: To examine the association of lifespan CR with dementia risk, taking brain pathologies into account.
Design, setting, and participants: This study used data from 2022 participants in the Rush Memory and Aging Project, an ongoing community-based cohort study with annual follow-up from 1997 to 2018 (mean follow-up, 6 years; maximum follow-up, 20 years). After excluding 420 individuals who had prevalent dementia, missing data on CR, or dropped out, 1602 dementia-free adults were identified at baseline and evaluated to detect incident dementia. During follow-up, 611 died and underwent autopsies. Data were analyzed from May to September 2018.
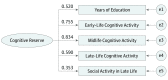
Exposures: Information on CR factors (education; early-life, midlife, and late-life cognitive activities; and social activities in late life) was obtained at baseline. Based on these factors, lifespan CR scores were captured using a latent variable from a structural equation model and was divided into tertiles (lowest, middle, and highest).
Main outcomes and measures: Dementia was diagnosed following international criteria. Neuropathologic evaluations for Alzheimer disease and other brain pathologies were performed in autopsied participants. The association of lifespan CR with dementia or brain pathologies was estimated using Cox regression models or logistic regression.
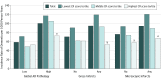
Results: Of the 1602 included participants, 1216 (75.9%) were women, and the mean (SD) age was 79.6 (7.5) years. During follow-up, 386 participants developed dementia (24.1%), including 357 participants with Alzheimer disease-related dementia (22.3%). The multiadjusted hazards ratios (HRs) of dementia were 0.77 (95% CI, 0.59-0.99) for participants in the middle CR score tertile and 0.61 (95% CI, 0.47-0.81) for those in the highest CR score tertile compared with those in the lowest CR score tertile. In autopsied participants, CR was not associated with most brain pathologies, and the association of CR with dementia remained significant after additional adjustment for brain pathologies (HR, 0.60; 95% CI, 0.42-0.86). The highest CR score tertile was associated with a reduction in dementia risk, even among participants with high Alzheimer disease pathology (HR, 0.57; 95% CI, 0.37-0.87) and any gross infarcts (HR, 0.34; 95% CI, 0.18-0.62).
Conclusions and relevance: High lifespan CR is associated with a reduction in dementia risk, even in the presence of high brain pathologies. Our findings highlight the importance of lifespan CR accumulation in dementia prevention.
Conflict of interest statement
Figures
Comment in
-
Lifespan Cognitive Reserve-A Secret to Coping With Neurodegenerative Pathology.JAMA Neurol. 2019 Oct 1;76(10):1145-1146. doi: 10.1001/jamaneurol.2019.2899. JAMA Neurol. 2019. PMID: 31609408 No abstract available.
Similar articles
-
Influence of Cognitive Reserve on Cognitive Trajectories: Role of Brain Pathologies.Neurology. 2021 Oct 26;97(17):e1695-e1706. doi: 10.1212/WNL.0000000000012728. Epub 2021 Sep 7. Neurology. 2021. PMID: 34493618 Free PMC article.
-
Association of lifespan cognitive reserve indicator with the risk of mild cognitive impairment and its progression to dementia.Alzheimers Dement. 2020 Jun;16(6):873-882. doi: 10.1002/alz.12085. Epub 2020 Apr 27. Alzheimers Dement. 2020. PMID: 32342664 Free PMC article.
-
Body Mass Index Trajectories Preceding Incident Mild Cognitive Impairment and Dementia.JAMA Psychiatry. 2022 Dec 1;79(12):1180-1187. doi: 10.1001/jamapsychiatry.2022.3446. JAMA Psychiatry. 2022. PMID: 36287554 Free PMC article.
-
Structural magnetic resonance imaging for the early diagnosis of dementia due to Alzheimer's disease in people with mild cognitive impairment.Cochrane Database Syst Rev. 2020 Mar 2;3(3):CD009628. doi: 10.1002/14651858.CD009628.pub2. Cochrane Database Syst Rev. 2020. PMID: 32119112 Free PMC article.
-
Use of Antihypertensives, Blood Pressure, and Estimated Risk of Dementia in Late Life: An Individual Participant Data Meta-Analysis.JAMA Netw Open. 2023 Sep 5;6(9):e2333353. doi: 10.1001/jamanetworkopen.2023.33353. JAMA Netw Open. 2023. PMID: 37698858 Free PMC article.
Cited by
-
A bidirectional relationship between cognitive reserve and cognition among older adults in a rural Chinese community: a cross-lagged design.Front Psychol. 2023 Dec 20;14:1297699. doi: 10.3389/fpsyg.2023.1297699. eCollection 2023. Front Psychol. 2023. PMID: 38192390 Free PMC article.
-
Association between Cognitive Reserve Indicator and Chronic Disease-Free Survival: A Large Community-Based Longitudinal Study.J Prev Alzheimers Dis. 2024;11(6):1712-1720. doi: 10.14283/jpad.2024.160. J Prev Alzheimers Dis. 2024. PMID: 39559882 Free PMC article.
-
Impaired Neurovascular Function Underlies Poor Neurocognitive Outcomes and Is Associated with Nitric Oxide Bioavailability in Congenital Heart Disease.Metabolites. 2022 Sep 19;12(9):882. doi: 10.3390/metabo12090882. Metabolites. 2022. PMID: 36144286 Free PMC article.
-
Dynamic functional connectivity patterns associated with dementia risk.Alzheimers Res Ther. 2022 May 23;14(1):72. doi: 10.1186/s13195-022-01006-7. Alzheimers Res Ther. 2022. PMID: 35606867 Free PMC article.
-
Harmonisation and Between-Country Differences of the Lifetime of Experiences Questionnaire in Older Adults.Front Aging Neurosci. 2021 Oct 14;13:740005. doi: 10.3389/fnagi.2021.740005. eCollection 2021. Front Aging Neurosci. 2021. PMID: 34720992 Free PMC article.
References
-
- Prince M, Acosta D, Ferri CP, et al. . Dementia incidence and mortality in middle-income countries, and associations with indicators of cognitive reserve: a 10/66 Dementia Research Group population-based cohort study. Lancet. 2012;380(9836):50-58. doi:10.1016/S0140-6736(12)60399-7 - DOI - PMC - PubMed

