"CHOICES": An acronym to aid in delineating potential causes of non-metabolic, non-infectious acute toxic leukoencephalopathy
- PMID: 31309133
- PMCID: PMC6607360
- DOI: 10.1016/j.ejro.2019.06.005
"CHOICES": An acronym to aid in delineating potential causes of non-metabolic, non-infectious acute toxic leukoencephalopathy
Erratum in
-
Erratum regarding missing Declaration of Competing Interest statements in previously published articles.Eur J Radiol Open. 2020 Dec 17;8:100308. doi: 10.1016/j.ejro.2020.100308. eCollection 2021. Eur J Radiol Open. 2020. PMID: 33364261 Free PMC article.
Abstract
Purpose: To describe non-metabolic, non-infectious etiologies of acute toxic leukoencephalopathy (ATL) on DWI MRI, and provide a useful acronym to remember them.
Material and methods: Our PACS archive was reviewed, yielding 185 patients with suspected ATL per MRI reports and clinical follow up; infectious or metabolic causes were excluded.
Result/discussion: The 87 included non-infectious, non-metabolic ATL patients' etiologies are represented by the acronym 'CHOICES': chemotherapy ('C',n = 34); heroin-induced ('H',n = 6), opioid analogues ('O',n = 14); immunosuppressant ('I',n = 11) or imidazole (n = 2); cocaine ('C',n = 1); environmental or ethanol abuse ('E',n = 5), splenial lesions ('S',n = 9), and 'other' (n = 5).
Conclusion: The "CHOICES" acronym delineates various toxic etiologies of ATL.
Keywords: ADEM, Acute disseminated encephalomyelitis; AEDs, Anti-epileptic drugs; AHE, Acute Hepatic/Hyperammonemic Encephalopathy; AHL, Acute hemorrhagic leukoencephalitis; ATL, Acute toxic leukoencephalopathy; Acute toxic leukoencephalopathy; CO, Carbon monoxide; Diffusion-Weighted imaging; EPM, Extrapontine myelinolysis; EtOH, Ethanol; HIE, Hypoxic-ischemic encephalopathy; LE, leukoencephalopathy; MBD, Marchiafava-Bignami Disease; MERS, Mild encephalitis/encephalopathy with reversible splenial lesion; NAWM, Normal-appearing white matter; ODS, Osmotic demyelination syndrome; PML, Progressive multifocal leukoencephalopathy; PRES, Posterior reversible encephalopathy syndrome; PVWM, Periventricular white matter; Periventricular white matter; RIS, Radiology information system; RSL, Reversible splenial lesions.
Figures







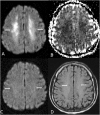








Similar articles
-
Potentially Reversible and Recognizable Acute Encephalopathic Syndromes: Disease Categorization and MRI Appearances.AJNR Am J Neuroradiol. 2020 Aug;41(8):1328-1338. doi: 10.3174/ajnr.A6634. Epub 2020 Jul 2. AJNR Am J Neuroradiol. 2020. PMID: 32616580 Free PMC article. Review.
-
Review of diffuse cortical injury on diffusion-weighted imaging in acutely encephalopathic patients with an acronym: "CRUMPLED".Eur J Radiol Open. 2018 Nov 9;5:194-201. doi: 10.1016/j.ejro.2018.10.004. eCollection 2018. Eur J Radiol Open. 2018. PMID: 30456218 Free PMC article.
-
Acute toxic leukoencephalopathy: potential for reversibility clinically and on MRI with diffusion-weighted and FLAIR imaging.AJR Am J Roentgenol. 2009 Jul;193(1):192-206. doi: 10.2214/AJR.08.1176. AJR Am J Roentgenol. 2009. PMID: 19542414
-
Concomitant Acute Toxic Leukoencephalopathy and Posterior Reversible Encephalopathy Syndrome.J Neuroimaging. 2018 Sep;28(5):535-541. doi: 10.1111/jon.12526. Epub 2018 May 24. J Neuroimaging. 2018. PMID: 29797465
-
Toxic leukoencephalopathy following fludarabine-associated hematopoietic cell transplantation.Biol Blood Marrow Transplant. 2011 Mar;17(3):300-8. doi: 10.1016/j.bbmt.2010.04.003. Epub 2010 Apr 24. Biol Blood Marrow Transplant. 2011. PMID: 20399878 Review.
Cited by
-
Potentially Reversible and Recognizable Acute Encephalopathic Syndromes: Disease Categorization and MRI Appearances.AJNR Am J Neuroradiol. 2020 Aug;41(8):1328-1338. doi: 10.3174/ajnr.A6634. Epub 2020 Jul 2. AJNR Am J Neuroradiol. 2020. PMID: 32616580 Free PMC article. Review.
-
Toxic leukoencephalopathy versus delayed post-hypoxic leukoencephalopathy after oral morphine sulphate overdose.BMJ Case Rep. 2023 Sep 27;16(9):e255291. doi: 10.1136/bcr-2023-255291. BMJ Case Rep. 2023. PMID: 37758656
-
Pediatric Acute Toxic Leukoencephalopathy: Prediction of the Clinical Outcome by FLAIR and DWI for Various Etiologies.AJNR Am J Neuroradiol. 2020 Aug;41(8):1517-1524. doi: 10.3174/ajnr.A6624. Epub 2020 Jul 2. AJNR Am J Neuroradiol. 2020. PMID: 32616577 Free PMC article.
-
Mild Encephalopathy/Encephalitis with Reversible Splenial Lesions after Amphetamine and Opioid Use.Intern Med. 2024 Oct 15;63(20):2857-2860. doi: 10.2169/internalmedicine.3002-23. Epub 2024 Mar 11. Intern Med. 2024. PMID: 38462522 Free PMC article.
-
Opioid-Induced Leukoencephalopathies: A Report of Two Cases.Case Rep Neurol. 2022 Feb 1;14(1):25-30. doi: 10.1159/000521410. eCollection 2022 Jan-Apr. Case Rep Neurol. 2022. PMID: 35221972 Free PMC article.
References
-
- Filley C.M., Kleinschmidt-DeMasters B.K. Toxic leukoencephalopathy. N. Engl. J. Med. 2001;345(6):425–432. - PubMed
-
- McKinney A.M. Acute toxic leukoencephalopathy: potential for reversibility clinically and on MRI with diffusion-weighted and FLAIR imaging. AJR Am. J. Roentgenol. 2009;193(1):192–206. - PubMed
-
- Beitinjaneh A. Toxic leukoencephalopathy following fludarabine-associated hematopoietic cell transplantation. Biol. Blood Marrow Transplant. 2011;17(3):300–308. - PubMed
-
- Keogh C.F. Neuroimaging features of heroin inhalation toxicity: "chasing the dragon". AJR Am. J. Roentgenol. 2003;180(3):847–850. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

