Longitudinal effect of nocturnal R-R intervals changes on cardiovascular outcome in a community-based cohort
- PMID: 31315880
- PMCID: PMC6661586
- DOI: 10.1136/bmjopen-2019-030559
Longitudinal effect of nocturnal R-R intervals changes on cardiovascular outcome in a community-based cohort
Abstract
Rationale: Sleep-disordered breathing (SDB) is strongly linked to adverse cardiovascular outcomes (cardiovascular diseases (CVD)). Whether heart rate changes measured by nocturnal R-R interval (RRI) dips (RRI dip index (RRDI)) adversely affect the CVD outcomes is unknown.
Objectives: To test whether nocturnal RRDI predicts CVD incidence and mortality in the Wisconsin Sleep Cohort study (WSCS), independent of the known effects of SDB on beat-to-beat variability.
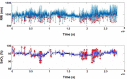
Methods: The study analysed electrocardiograph obtained from polysomnography study to assess the nocturnal total RRDI (the number of RRI dips divided by the total recording time) and sleep RRDI (the number of RRI dips divided by total sleep time). A composite CVD risk as a function of total and sleep RRDI was estimated by Cox proportional hazards in the WSCS.
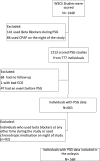
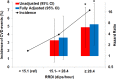
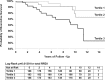
Results: The study sample consisted of 569 participants from the WSCS with no prior CVD at baseline were followed up for up to 15 years. Nocturnal total RRDI (10-unit change) was associated with composite CVD event(s) (HR, 1.24 per 10-unit increment in RRDI (95% CI 1.10 to 1.39), p<0.001). After adjusting for demographic factors (age 58±8 years old; 53% male; and body mass index 31±7 kg/m2), and apnoea-hypopnoea index (AHI 4%), individuals with highest total nocturnal RRDI category (≥28 vs<15 dips/hour) had a significant HR for increased incidence of CVD and mortality of 7.4(95% CI 1.97 to 27.7), p=0.003). Sleep RRDI was significantly associated with new-onset CVD event(s) (HR, 1.21 per 10-unit increment in RRDI (95% CI 1.09 to 1.35), p<0.001) which remained significant after adjusting for demographic factors, AHI 4%, hypoxemia and other comorbidities.
Conclusion: Increased nocturnal RRDI predicts cardiovascular mortality and morbidity, independent of the known effects of SDB on beat-to-beat variability. The frequency of RRDI is higher in men than in women, and is significantly associated with new-onset CVD event(s) in men but not in women.
Keywords: cardiac epidemiology; cardiovascular disease; epidemiology; heart rate; sleep medicine.
© Author(s) (or their employer(s)) 2019. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures

References
-
- Somers VK, White DP, Amin R, et al. Sleep apnea and cardiovascular disease: an American Heart Association/american College Of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council On Cardiovascular Nursing. In collaboration with the National Heart, Lung, and Blood Institute National Center on Sleep Disorders Research (National Institutes of Health). Circulation 2008;118:1080–111. 10.1161/CIRCULATIONAHA.107.189375 - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
