Avatar-Based Patient Monitoring With Peripheral Vision: A Multicenter Comparative Eye-Tracking Study
- PMID: 31317870
- PMCID: PMC6668297
- DOI: 10.2196/13041
Avatar-Based Patient Monitoring With Peripheral Vision: A Multicenter Comparative Eye-Tracking Study
Abstract
Background: Continuous patient monitoring has been described by the World Health Organization as extremely important and is widely used in anesthesia, intensive care medicine, and emergency medicine. However, current state-of-the-art number- and waveform-based monitoring does not ideally support human users in acquiring quick, confident interpretations with low cognitive effort, and there are additional problematic aspects such as alarm fatigue. We developed a visualization technology (Visual Patient), specifically designed to help caregivers gain situation awareness quickly, which presents vital sign information in the form of an animated avatar of the monitored patient. We suspected that because of the way it displays the information as large, colorful, moving graphic objects, caregivers might be able to perform patient monitoring using their peripheral vision, which may facilitate quicker detection of anomalies, independently of acoustic alarms.
Objective: In this study, we tested the hypothesis that avatar-based monitoring, when observed with peripheral vision only, increases the number of perceptible changes in patient status as well as caregivers' perceived diagnostic confidence compared with a high-fidelity simulation of conventional monitoring, when observed with peripheral vision only.
Methods: We conducted a multicenter comparative study with a within-participant design in which anesthesiologists with their peripheral field of vision looked at 2 patient-monitoring scenarios and tried to identify changes in patient status. To ensure the best possible experimental conditions, we used an eye tracker, which recorded the eye movements of the participants and confirmed that they only looked at the monitoring scenarios with their peripheral vision.
Results: Overall, 30 participants evaluated 18 different patient status changes with each technology (avatar and conventional patient monitoring). With conventional patient monitoring, participants could only detect those 3 changes in patient status that are associated with a change in the auditory pulse tone display, that is, tachycardia (faster beeping), bradycardia (slower beeping), and desaturation (lower pitch of beeping). With the avatar, the median number of detected vital sign changes quadrupled from 3 to 12 (P<.001) in scenario 1, and more than doubled from 3 to 8 (P<.001) in scenario 2. Median perceived diagnostic confidence was confident for both scenarios with the avatar and unconfident in scenario 1 (P<.001), and very unconfident in scenario 2 (P=.024) with conventional monitoring.
Conclusions: This study introduces the concept of peripheral vision monitoring. The test performed showed clearly that an avatar-based display is superior to a standard numeric display for peripheral vision. Avatar-based monitoring could potentially make much more of the patient monitoring information available to caregivers for longer time periods per case. Our results indicate that the optimal information transmission would consist of a combination of auditory and avatar-based monitoring.
Keywords: anesthesia; computers; critical care; diagnosis; patient monitoring; perception; situation awareness; vision.
©Juliane Pfarr, Michael T Ganter, Donat R Spahn, Christoph B Noethiger, David W Tscholl. Originally published in the Journal of Medical Internet Research (http://www.jmir.org), 17.07.2019.
Conflict of interest statement
Conflicts of Interest: The authors DWT, DRS, and CBN are in a joint development agreement with the monitoring manufacturer Philips Healthcare (Koninklijke Philips NV). Within the framework of this cooperation, a monitoring system based on an avatar will be developed. Within the framework of licensing the technology via the University, the authors DWT and CBN might receive royalties as designated inventors in the event of a successful product release.
Figures


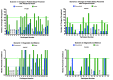
References
-
- WHO Guidelines for Safe Surgery 2009: Safe Surgery Saves Lives. Geneva: World Health Organization; 2009. - PubMed
-
- Moller JT, Jensen PF, Johannessen NW, Espersen K. Hypoxaemia is reduced by pulse oximetry monitoring in the operating theatre and in the recovery room. Br J Anaesth. 1992 Feb;68(2):146–50. doi: 10.1093/bja/68.2.146. https://linkinghub.elsevier.com/retrieve/pii/S0007-0912(17)46722-5 - DOI - PubMed
-
- Moller JT, Johannessen NW, Espersen K, Ravlo O, Pedersen BD, Jensen PF, Rasmussen NH, Rasmussen LS, Pedersen T, Cooper JB. Randomized evaluation of pulse oximetry in 20,802 patients: II. Perioperative events and postoperative complications. Anesthesiology. 1993 Mar;78(3):445–53. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

