The prognostic role of platelet-to-lymphocyte ratio in patients with acute heart failure: A cohort study
- PMID: 31337846
- PMCID: PMC6650439
- DOI: 10.1038/s41598-019-47143-2
The prognostic role of platelet-to-lymphocyte ratio in patients with acute heart failure: A cohort study
Abstract
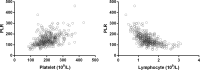
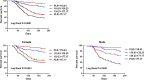
Identification of rapid, inexpensive, and reliable prognostic factors can improve survival estimation and guide healthcare in patients with acute heart failure (AHF). In this study, we aimed to determine the prognostic value of the platelet-to-lymphocyte ratio (PLR) in patients with AHF. A total of 443 patients from two hospitals met the inclusion criteria from January 2010 to December 2017. Univariate and multivariate Cox analyses were performed to determine the association of PLR with survival. All-cause mortality was analysed using the Kaplan-Meier method. The 6-month survival rate for patients according to PLR quartiles (<110.63, 110.63-139.23, 139.23-177.17, and >177.17) were 90.09%, 76.79%, 50.07%, and 37.27%, respectively (p < 0.001). Univariate analysis identified high PLR (>110.63), old age (≥73 years), smoking habit, low estimated glomerular filtration rate (<57), and high platelet count (≥198 × 109/l) as poor prognostic factors for survival. In the multivariate analysis, after adjusting for confounding factors, the third (hazard ratio [HR] = 3.118, 95% confidence interval [CI] = 1.668-5.386, p < 0.001) and fourth (HR = 2.437, 95% CI = 1.302-3.653, p < 0.001) quartiles of PLR were identified as independent prognostic factors in patients with AHF. A higher PLR was associated with poor clinical outcomes in patients with AHF and might be a novel marker in AHF management.
Conflict of interest statement
The authors declare no competing interests.
Figures

References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

