Impact of the 2015 Middle East Respiratory Syndrome Outbreak on Emergency Care Utilization and Mortality in South Korea
- PMID: 31347336
- PMCID: PMC6660446
- DOI: 10.3349/ymj.2019.60.8.796
Impact of the 2015 Middle East Respiratory Syndrome Outbreak on Emergency Care Utilization and Mortality in South Korea
Abstract
Purpose: In May 2015, South Korea experienced an epidemic of Middle East respiratory syndrome (MERS). This study investigated the impacts of MERS epidemic on emergency care utilization and mortality in South Korea.
Materials and methods: A natural experimental study was conducted using healthcare utilization and mortality data of the entire Korean population. The number of monthly emergency room (ER) visits was investigated to identify changes in emergency care utilization during the MERS epidemic; these trends were also examined according to patients' demographic factors, disease severity, and region. Deaths within 7 days after visiting an ER were analyzed to evaluate the impact of the reduction in ER visits on mortality.
Results: The number of ER visits during the peak of the MERS epidemic (June 2015) decreased by 33.1% compared to the average figures from June 2014 and June 2016. The decrease was observed in all age, sex, and income groups, and was more pronounced for low-acuity diseases (acute otitis media: 53.0%; upper respiratory infections: 45.2%) than for high-acuity diseases (myocardial infarctions: 14.0%; ischemic stroke: 16.6%). No substantial changes were detected for the highest-acuity diseases, with increases of 3.5% for cardiac arrest and 2.4% for hemorrhagic stroke. The number of deaths within 7 days of an ER visit did not change significantly.
Conclusion: During the MERS epidemic, the number of ER visits decreased in all age, sex, and socioeconomic groups, and decreased most sharply for low-acuity diseases. Nonetheless, there was no significant change in deaths after emergency care.
Keywords: Middle East respiratory syndrome (MERS); communicable diseases, emerging; disaster planning; emergency service, hospital.
© Copyright: Yonsei University College of Medicine 2019.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
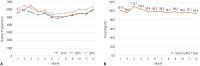
Figures


Similar articles
-
The Impact of Middle East Respiratory Syndrome Outbreak on Trends in Emergency Department Utilization Patterns.J Korean Med Sci. 2017 Oct;32(10):1576-1580. doi: 10.3346/jkms.2017.32.10.1576. J Korean Med Sci. 2017. PMID: 28875599 Free PMC article.
-
Mortality Risk Factors for Middle East Respiratory Syndrome Outbreak, South Korea, 2015.Emerg Infect Dis. 2015 Nov;21(11):2088-90. doi: 10.3201/eid2111.151231. Emerg Infect Dis. 2015. PMID: 26488869 Free PMC article.
-
Middle East Respiratory Syndrome Coronavirus Superspreading Event Involving 81 Persons, Korea 2015.J Korean Med Sci. 2015 Nov;30(11):1701-5. doi: 10.3346/jkms.2015.30.11.1701. Epub 2015 Oct 16. J Korean Med Sci. 2015. PMID: 26539018 Free PMC article.
-
Factors Influencing the Response to Infectious Diseases: Focusing on the Case of SARS and MERS in South Korea.Int J Environ Res Public Health. 2019 Apr 22;16(8):1432. doi: 10.3390/ijerph16081432. Int J Environ Res Public Health. 2019. PMID: 31013648 Free PMC article.
-
MERS transmission and risk factors: a systematic review.BMC Public Health. 2018 May 2;18(1):574. doi: 10.1186/s12889-018-5484-8. BMC Public Health. 2018. PMID: 29716568 Free PMC article.
Cited by
-
Operating Protocols of a Community Treatment Center for Isolation of Patients with Coronavirus Disease, South Korea.Emerg Infect Dis. 2020 Oct;26(10):2329-2337. doi: 10.3201/eid2610.201460. Epub 2020 Jun 22. Emerg Infect Dis. 2020. PMID: 32568665 Free PMC article.
-
Demographics and clinical characteristics of hospitalised patients under investigation for COVID-19 with an initial negative SARS-CoV-2 PCR test result.Afr J Emerg Med. 2021 Dec;11(4):429-435. doi: 10.1016/j.afjem.2021.09.002. Epub 2021 Sep 27. Afr J Emerg Med. 2021. PMID: 34603945 Free PMC article.
-
Preparedness and Response to Pediatric COVID-19 in European Emergency Departments: A Survey of the REPEM and PERUKI Networks.Ann Emerg Med. 2020 Dec;76(6):788-800. doi: 10.1016/j.annemergmed.2020.05.018. Epub 2020 May 15. Ann Emerg Med. 2020. PMID: 32419713 Free PMC article.
-
Pre-existing cerebrovascular disease and poor outcomes of COVID-19 hospitalized patients: a meta-analysis.J Neurol. 2021 Jan;268(1):240-247. doi: 10.1007/s00415-020-10141-w. Epub 2020 Aug 8. J Neurol. 2021. PMID: 32770412 Free PMC article.
-
Implications of COVID-19 in Neurological Disorders.J Neurol Res. 2020 Oct;10(5):160-163. doi: 10.14740/jnr617. Epub 2020 Aug 25. J Neurol Res. 2020. PMID: 33984089 Free PMC article. Review.
References
-
- Fagbuyi DB, Brown KM, Mathison DJ, Kingsnorth J, Morrison S, Saidinejad M, et al. A rapid medical screening process improves emergency department patient flow during surge associated with novel H1N1 influenza virus. Ann Emerg Med. 2011;57:52–59. - PubMed
-
- Costello BE, Simon HK, Massey R, Hirsh DA. Pandemic H1N1 influenza in the pediatric emergency department: a comparison with previous seasonal influenza outbreaks. Ann Emerg Med. 2010;56:643–648. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

