Accuracy of chest auscultation in detecting abnormal respiratory mechanics in the immediate postoperative period after cardiac surgery
- PMID: 31365614
- PMCID: PMC6715162
- DOI: 10.1590/1806-3713/e20180032
Accuracy of chest auscultation in detecting abnormal respiratory mechanics in the immediate postoperative period after cardiac surgery
Abstract
Objective: To investigate the accuracy of chest auscultation in detecting abnormal respiratory mechanics.
Methods: We evaluated 200 mechanically ventilated patients in the immediate postoperative period after cardiac surgery. We assessed respiratory system mechanics - static compliance of the respiratory system (Cst,rs) and respiratory system resistance (R,rs) - after which two independent examiners, blinded to the respiratory system mechanics data, performed chest auscultation.
Results: Neither decreased/abolished breath sounds nor crackles were associated with decreased Cst,rs (≤ 60 mL/cmH2O), regardless of the examiner. The overall accuracy of chest auscultation was 34.0% and 42.0% for examiners A and B, respectively. The sensitivity and specificity of chest auscultation for detecting decreased/abolished breath sounds or crackles were 25.1% and 68.3%, respectively, for examiner A, versus 36.4% and 63.4%, respectively, for examiner B. Based on the judgments made by examiner A, there was a weak association between increased R,rs (≥ 15 cmH2O/L/s) and rhonchi or wheezing (ϕ = 0.31, p < 0.01). The overall accuracy for detecting rhonchi or wheezing was 89.5% and 85.0% for examiners A and B, respectively. The sensitivity and specificity for detecting rhonchi or wheezing were 30.0% and 96.1%, respectively, for examiner A, versus 10.0% and 93.3%, respectively, for examiner B.
Conclusions: Chest auscultation does not appear to be an accurate diagnostic method for detecting abnormal respiratory mechanics in mechanically ventilated patients in the immediate postoperative period after cardiac surgery.
Objetivo:: Investigar a acurácia da ausculta torácica na detecção de mecânica respiratória anormal.
Métodos:: Foram avaliados 200 pacientes sob ventilação mecânica no pós-operatório imediato de cirurgia cardíaca. Foi avaliada a mecânica do sistema respiratório - complacência estática do sistema respiratório (Cest,sr) e resistência do sistema respiratório (R,sr) - e, em seguida, dois examinadores independentes, que desconheciam os dados referentes à mecânica do sistema respiratório, realizaram a ausculta torácica.
Resultados:: Nem murmúrio vesicular diminuído/abolido nem crepitações foram associados à Cest,sr reduzida (≤ 60 ml/cmH2O), independentemente do examinador. A acurácia global da ausculta torácica foi de 34,0% e 42,0% para os examinadores A e B, respectivamente. A sensibilidade e a especificidade da ausculta torácica para a detecção de murmúrio vesicular diminuído/abolido e/ou crepitações foi de 25,1% e 68,3%, respectivamente, para o examinador A, versus 36,4% e 63,4%, respectivamente, para o examinador B. Com base nos julgamentos feitos pelo examinador A, houve uma fraca associação entre R,sr aumentada (≥ 15 cmH2O/l/s) e roncos e/ou sibilos (ϕ = 0,31, p < 0,01). A acurácia global para a detecção de roncos e/ou sibilos foi de 89,5% e 85,0% para os examinadores A e B, respectivamente. A sensibilidade e a especificidade para a detecção de roncos e/ou sibilos foi de 30,0% e 96,1%, respectivamente, para o examinador A, versus 10,0% e 93,3%, respectivamente, para o examinador B.
Conclusões:: A ausculta torácica não parece ser um método diagnóstico acurado para a detecção de mecânica respiratória anormal em pacientes sob ventilação mecânica no pós-operatório imediato de cirurgia cardíaca.
Figures
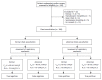

References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

