Imaging in chronic pancreatitis: State of the art review
- PMID: 31367093
- PMCID: PMC6639861
- DOI: 10.4103/ijri.IJRI_484_18
Imaging in chronic pancreatitis: State of the art review
Abstract
Chronic pancreatitis (CP) is an important gastrointestinal cause of morbidity worldwide. It can severely impair the quality of life besides life-threatening acute and long-term complications. Pain and pancreatic exocrine insufficiency (leading to malnutrition) impact the quality of life. Acute complications include pseudocysts, pancreatic ascites, and vascular complications. Long-term complications are diabetes mellitus and pancreatic cancer. Early diagnosis of CP is crucial to alter the natural course of the disease. However, majority of the cases are diagnosed in the advanced stage. The role of various imaging techniques in the diagnosis of CP is discussed in this review.
Keywords: Chronic pancreatitis; diagnosis; imaging.
Conflict of interest statement
There are no conflicts of interest.
Figures
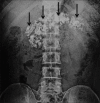
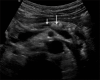
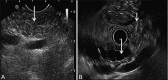
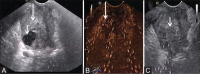
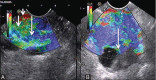
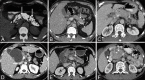
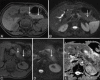
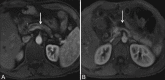
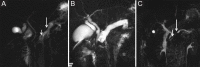
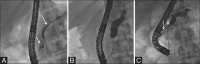
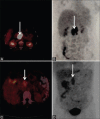

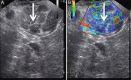
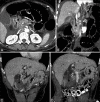
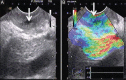
References
-
- De Backer AI, Mortele KJ, Ros RR, Vanbeckevoort D, Vanschoubroeck I, De Keulenaer B. Chronic pancreatitis: Diagnostic role of computed tomography and magnetic resonance imaging. JBR-BTR. 2002;85:304–10. - PubMed
-
- Sharma R, Kandasamy D. Imaging in chronic pancreatitis. Pancreapedia Exocrine Pancreas Knowl Base. 2015
-
- Perez-Johnston R, Sainani NI, Sahani DV. Imaging of chronic pancreatitis (including groove and autoimmune pancreatitis) Radiol Clin North Am. 2012;50:447–66. - PubMed
-
- Siddiqi AJ, Miller F. Chronic pancreatitis: Ultrasound, computed tomography, and magnetic resonance imaging features. Semin Ultrasound CT MRI. 2007;28:384–94. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

