Predictors of postoperative outcomes in infants with low birth weight undergoing congenital heart surgery: a retrospective observational study
- PMID: 31371972
- PMCID: PMC6628950
- DOI: 10.2147/TCRM.S206147
Predictors of postoperative outcomes in infants with low birth weight undergoing congenital heart surgery: a retrospective observational study
Abstract
Background: Despite improvements in neonatal cardiac surgery and postoperative care, hospitalized death for infants with low birth weight remains high.
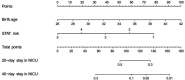
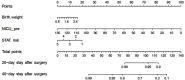
Objective: This study sought to identify predictors of postoperative outcomes in low-birth-weight infants undergoing congenital heart surgery and establish nomograms to predict postoperative intensive-care unit (ICU) stay.
Methods: From June 2009 to June 2018, a retrospective review of 114 infants with low birth weight (≤2.5 kg) undergoing congenital heart surgery was conducted at Guangdong Provincial People's Hospital. Purely surgical ligation of patent ductus arteriosus was excluded from this study. A total of 26 clinical variables were chosen for univariate, multivariate, and Cox regression analysis, and 14 variables were analyzed as predictors of postoperative outcomes. Nomograms were established to predict risk of postoperative cardiac ICU (CICU) stay, postoperative neonatal ICU (NICU) stay, and total ICU length of stay in infants with cardiac diseases.
Results: Two variables were independent predictors in multiple logistic regression analysis of hospitalized death: operation weight and Society of Thoracic Surgeons-European Association for Cardio-Thoracic Surgery (STAT) risk categories. Six variables were independent predictors in the Cox model of postoperative ICU length of stay, including sex, prematurity, birth weight, preoperative stay time in NICU, diagnostic classification, and STAT risk categories. We calculated concordance-index values to estimate the discriminative ability of models of risk of postoperative CICU stay, postoperative NICU stay, and total ICU length of stay, with values of 0.758 (95% CI 0.696-0.820), 0.604 (95% CI 0.525-0.682), and 0.716 (95% CI 0.657-0.776), which indicated the possibility of true-positive results.
Conclusion: Our findings might help clinicians predict postoperative outcomes and optimize therapeutic strategies.
Keywords: congenital heart disease; low birth weight; neonatal cardiac surgery; nomogram; outcome prognosis; predictive tools.
Conflict of interest statement
JZ received funding from Guangdong Project of Science and Technology (2017A070701013 and 2017B090904034). SW received funding from the Natural Science Foundation of Guangdong Province (2018A030313535). The authors report no other conflicts of interest in this work.
Figures

References
-
- Kramer HH, Trampisch HJ, Rammos S, et al. Birth weight of children with congenital heart disease. Eur J Pediatr. 1990;149:752–757. - PubMed
LinkOut - more resources
Full Text Sources

