Improving Daytime Functioning, Work Performance, and Quality of Life in Postmenopausal Women With Insomnia: Comparing Cognitive Behavioral Therapy for Insomnia, Sleep Restriction Therapy, and Sleep Hygiene Education
- PMID: 31383238
- PMCID: PMC6622507
- DOI: 10.5664/jcsm.7882
Improving Daytime Functioning, Work Performance, and Quality of Life in Postmenopausal Women With Insomnia: Comparing Cognitive Behavioral Therapy for Insomnia, Sleep Restriction Therapy, and Sleep Hygiene Education
Abstract
Study objectives: Insomnia is a chief complaint among postmenopausal women, and insomnia impairs daytime functioning and reduces quality of life. Recent evidence supports the efficacy of cognitive behavioral therapy for insomnia (CBTI) for menopausal insomnia, but it remains unclear whether treating insomnia improves daytime function in this population. This study evaluated whether CBTI improves daytime fatigue, energy, self-reported sleepiness, work productivity, and quality of life in postmenopausal women with insomnia, and whether sleep restriction therapy (SRT)-a single component of CBTI-is equally efficacious.
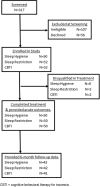
Methods: Single-site, randomized control trial. One hundred fifty postmenopausal women (56.44 ± 5.64 years) with perimenopausal or postmenopausal onset or exacerbation of chronic insomnia were randomized to 3 treatment conditions: sleep hygiene education control (SHE), SRT, and CBTI. Blinded assessments were performed at pretreatment, posttreatment, and 6-month follow-up.
Results: CBTI and SRT produced moderate-to-large improvements in fatigue, energy, sleepiness, and work function at posttreatment and 6 months later. The CBTI group reported better quality of life as indicated by substantial improvements in emotional wellbeing and resiliency to physical and emotional problems, whereas the SRT and SHE groups only showed improvements in resiliency to physical problems. Pain complaints decreased as sleep improved but were not associated with specific treatment conditions. Similarly, insomnia remitters reported fewer daytime and nighttime hot flashes, although reductions were not associated with any specific treatment.
Conclusions: CBTI and SRT are efficacious options for postmenopausal women with chronic insomnia. Both interventions improve daytime function, quality of life, and work performance, although CBTI produces superior results including the added benefit of improved emotional health.
Clinical trial registration: Registry: ClinicalTrials.gov; Title: Behavioral Treatment of Menopausal Insomnia; Sleep and Daytime Outcomes; Identifier: NCT01933295; URL: https://clinicaltrials.gov/ct2/show/record/NCT01933295.
Keywords: fatigue; hot flashes; menopause; quality of life; sleep; sleepiness; work impairment.
Copyright © 2019 American Academy of Sleep Medicine. All rights reserved.
Figures
Similar articles
-
Objective sleep disturbance is associated with poor response to cognitive and behavioral treatments for insomnia in postmenopausal women.Sleep Med. 2020 Sep;73:82-92. doi: 10.1016/j.sleep.2020.04.024. Epub 2020 May 7. Sleep Med. 2020. PMID: 32799029 Free PMC article. Clinical Trial.
-
Treating insomnia improves depression, maladaptive thinking, and hyperarousal in postmenopausal women: comparing cognitive-behavioral therapy for insomnia (CBTI), sleep restriction therapy, and sleep hygiene education.Sleep Med. 2019 Mar;55:124-134. doi: 10.1016/j.sleep.2018.11.019. Epub 2018 Dec 28. Sleep Med. 2019. PMID: 30785053 Free PMC article. Clinical Trial.
-
Treating chronic insomnia in postmenopausal women: a randomized clinical trial comparing cognitive-behavioral therapy for insomnia, sleep restriction therapy, and sleep hygiene education.Sleep. 2019 Feb 1;42(2):zsy217. doi: 10.1093/sleep/zsy217. Sleep. 2019. PMID: 30481333 Free PMC article. Clinical Trial.
-
Is cognitive behavioral therapy for insomnia more cost-effective? New-perspective on economic evaluations: a systematic review and meta-analysis.Sleep. 2024 Aug 14;47(8):zsae122. doi: 10.1093/sleep/zsae122. Sleep. 2024. PMID: 38795362
-
Internet-Delivered Cognitive Behavioral Therapy for Insomnia: Tailoring Cognitive Behavioral Therapy for Insomnia for Patients with Chronic Insomnia.Sleep Med Clin. 2020 Jun;15(2):117-131. doi: 10.1016/j.jsmc.2020.02.001. Sleep Med Clin. 2020. PMID: 32386688 Review.
Cited by
-
Advances in the Treatment of Chronic Insomnia: A Narrative Review of New Nonpharmacologic and Pharmacologic Therapies.Neuropsychiatr Dis Treat. 2021 Aug 6;17:2549-2566. doi: 10.2147/NDT.S297504. eCollection 2021. Neuropsychiatr Dis Treat. 2021. PMID: 34393484 Free PMC article. Review.
-
Cultural adaptations of psychological interventions for prevalent sleep disorders and sleep disturbances: A systematic review of randomized controlled trials in the United States.Sleep Med Rev. 2021 Apr;56:101455. doi: 10.1016/j.smrv.2021.101455. Epub 2021 Feb 9. Sleep Med Rev. 2021. PMID: 33735638 Free PMC article.
-
Acupuncture combined with cognitive-behavioural therapy for insomnia (CBT-I) in patients with insomnia: study protocol for a randomised controlled trial.BMJ Open. 2022 Dec 30;12(12):e063442. doi: 10.1136/bmjopen-2022-063442. BMJ Open. 2022. PMID: 36585134 Free PMC article.
-
[Exploring the therapeutic mechanism of Liuwei Suanzao decoction for perimenopausal insomnia based on network pharmacology and animal experiments].Nan Fang Yi Ke Da Xue Xue Bao. 2023 Sep 20;43(9):1536-1547. doi: 10.12122/j.issn.1673-4254.2023.09.11. Nan Fang Yi Ke Da Xue Xue Bao. 2023. PMID: 37814868 Free PMC article. Chinese.
-
Objective sleep disturbance is associated with poor response to cognitive and behavioral treatments for insomnia in postmenopausal women.Sleep Med. 2020 Sep;73:82-92. doi: 10.1016/j.sleep.2020.04.024. Epub 2020 May 7. Sleep Med. 2020. PMID: 32799029 Free PMC article. Clinical Trial.
References
-
- Blumel JE, Castelo-Branco C, Binfa L, et al. Quality of life after the menopause: a population study. Maturitas. 2000;34(1):17–23. - PubMed
-
- Williams RE, Levine KB, Kalilani L, Lewis J, Clark RV. Menopause-specific questionnaire assessment in US population-based study shows negative impact on health-related quality of life. Maturitas. 2009;62(2):153–159. - PubMed
-
- Juang KD, Wang SJ, Lu SR, Lee SJ, Fuh JL. Hot flashes are associated with psychological symptoms of anxiety and depression in peri-and post-but not premenopausal women. Maturitas. 2005;52(2):119–126. - PubMed
-
- Porter M, Penney GC, Russell D, Russell E, Templeton A. A population based survey of women's experience of the menopause. Br J Obstet Gynaecol. 1996;103(10):1025–1028. - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical