Hospitalist-Operated Compression Ultrasonography: a Point-of-Care Ultrasound Study (HOCUS-POCUS)
- PMID: 31388904
- PMCID: PMC6816719
- DOI: 10.1007/s11606-019-05120-5
Hospitalist-Operated Compression Ultrasonography: a Point-of-Care Ultrasound Study (HOCUS-POCUS)
Abstract
Background: Venous thromboembolism includes deep vein thrombosis (DVT) and pulmonary embolism. Compression ultrasonography is the most common way to evaluate DVT and is typically performed by sonographers and interpreted by radiologists. Yet there is evidence that ultrasound examinations can be safely and accurately performed by clinicians at the bedside.
Objective: To measure the operating characteristics of hospital medicine providers performing point-of-care ultrasound (POCUS) for evaluation of DVT.
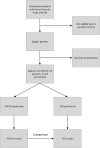
Design: This is a prospective cohort study enrolling a convenience sample of patients. Hospital medicine providers performed POCUS for DVT and the results were compared with the corresponding formal vascular study (FVS) interpreted by radiologists.
Participants: Hospitalized non-ICU patients at four tertiary care hospitals for whom a DVT ultrasound was ordered.
Main measures: The primary outcomes were the sensitivity, specificity, and predictive values of the POCUS compression ultrasound compared with a FVS. The secondary outcome was the elapsed time between order and the POCUS study compared with the time the FVS was ordered to when the formal radiology report was finalized.
Key results: One hundred twenty-five limbs from 73 patients were scanned. The prevalence of DVT was 6.4% (8/125). The sensitivity of POCUS for DVT was 100% (95% CI 74-100%) and specificity was 95.8% (95% CI 91-98%) with a positive predictive value of 61.5% (95% CI 35-84%) and a negative predictive value of 100% (95% CI 98-100%). The median time from order to POCUS completion was 5.8 h versus 11.5 h median time from order until the radiology report was finalized (p = 0.001).
Conclusion: Hospital medicine providers can perform compression-only POCUS for DVT on inpatients with accuracy similar to other specialties and settings, with results available sooner than radiology. The observed prevalence of DVT was lower than expected. POCUS may be reliable in excluding DVT but further study is required to determine how to incorporate a positive POCUS DVT result into clinical practice.
Keywords: hospitalists; thromboembolism; ultrasonography.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Similar articles
-
Diagnostic value of point-of-care ultrasound in deep vein thrombosis in the emergency department.J Clin Ultrasound. 2020 Nov;48(9):527-531. doi: 10.1002/jcu.22892. Epub 2020 Jul 9. J Clin Ultrasound. 2020. PMID: 32643227
-
Resident performed two-point compression ultrasound is inadequate for diagnosis of deep vein thrombosis in the critically III.J Thromb Thrombolysis. 2014 Apr;37(3):298-302. doi: 10.1007/s11239-013-0945-5. J Thromb Thrombolysis. 2014. PMID: 23722715 Clinical Trial.
-
Mistakes and Pitfalls Associated with Two-Point Compression Ultrasound for Deep Vein Thrombosis.West J Emerg Med. 2016 Mar;17(2):201-8. doi: 10.5811/westjem.2016.1.29335. Epub 2016 Mar 2. West J Emerg Med. 2016. PMID: 26973753 Free PMC article.
-
Point-of-Care Ultrasound for Bedside Diagnosis of Lower Extremity DVT.Chest. 2021 Nov;160(5):1853-1863. doi: 10.1016/j.chest.2021.07.010. Epub 2021 Jul 13. Chest. 2021. PMID: 34270964 Review.
-
Ultrasound Performed by Emergency Physicians for Deep Vein Thrombosis: A Systematic Review.West J Emerg Med. 2024 Mar;25(2):282-290. doi: 10.5811/westjem.18125. West J Emerg Med. 2024. PMID: 38596931 Free PMC article.
Cited by
-
Hematological Abnormalities in COVID-19: A Narrative Review.Am J Trop Med Hyg. 2021 Feb 19;104(4):1188-1201. doi: 10.4269/ajtmh.20-1536. Am J Trop Med Hyg. 2021. PMID: 33606667 Free PMC article. Review.
-
Management of Thrombotic Complications in COVID-19: An Update.Drugs. 2020 Oct;80(15):1553-1562. doi: 10.1007/s40265-020-01377-x. Drugs. 2020. PMID: 32803670 Free PMC article. Review.
-
Clinical Features and Management of COVID-19-Associated Hypercoagulability.Card Electrophysiol Clin. 2022 Mar;14(1):41-52. doi: 10.1016/j.ccep.2021.10.005. Epub 2021 Oct 30. Card Electrophysiol Clin. 2022. PMID: 35221084 Free PMC article. Review.
-
Design and comparison of a hybrid to a traditional in-person point-of-care ultrasound course.Ultrasound J. 2022 Mar 12;14(1):12. doi: 10.1186/s13089-022-00261-x. Ultrasound J. 2022. PMID: 35278145 Free PMC article.
-
The Use of Point-of-Care Ultrasound (POCUS) in the Diagnosis of Deep Vein Thrombosis.J Clin Med. 2021 Aug 30;10(17):3903. doi: 10.3390/jcm10173903. J Clin Med. 2021. PMID: 34501350 Free PMC article. Review.
References
-
- DHHS. The surgeon general’s call to action to prevent deep vein thrombosis and pulmonary embolism. 2008. http://www.ncbi.nlm.nih.gov/pubmed/20669525. Accessed 2/9/2019. - PubMed
-
- Kearon C, Akl EA, Comerota AJ, et al. Antithrombotic Therapy for VTE Disease: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012;141(2 Suppl):e419S–e496S. doi: 10.1378/chest.11-2301. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical