Energy Intake Requirements in Pregnancy
- PMID: 31390778
- PMCID: PMC6723706
- DOI: 10.3390/nu11081812
Energy Intake Requirements in Pregnancy
Abstract
Energy intake requirements in pregnancy match the demands of resting metabolism, physical activity, and tissue growth. Energy balance in pregnancy is, therefore, defined as energy intake equal to energy expenditure plus energy storage. A detailed understanding of these components and their changes throughout gestation can inform energy intake recommendations for minimizing the risk of poor pregnancy outcomes. Energy expenditure is the sum of resting and physical activity-related expenditure. Resting metabolic rate increases during pregnancy as a result of increased body mass, pregnancy-associated physiological changes, i.e., cardiac output, and the growing fetus. Physical activity is extremely variable between women and may change over the course of pregnancy. The requirement for energy storage depends on maternal pregravid body size. For optimal pregnancy outcomes, women with low body weight require more fat mass accumulation than women with obesity, who do not require to accumulate fat mass at all. Given the high energy density of fat mass, these differences affect energy intake requirements for a healthy pregnancy greatly. In contrast, the energy stored in fetal and placental tissues is comparable between all women and have small impact on energy requirements. Different prediction equations have been developed to quantify energy intake requirements and we provide a brief review of the strengths and weaknesses and discuss their application for healthy management of weight gain in pregnant women.
Keywords: energy expenditure; energy intake; fetal development; metabolic rate; physical activity; pregnancy.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures
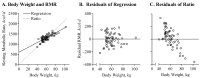
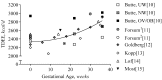

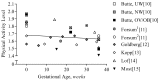
References
-
- Institute of Medicine (US) and National Research Council (US) Committee to Reexamine IOM Pregnancy Weight Guidelines . Determining optimal weight gain. In: Rasmussen K.M., Yaktine A.L., editors. Weight Gain during Pregnancy: Reexamining the Guidelines. National Academies Press; Washington, DC, USA: 2009. - PubMed
-
- Laitinen J., Jaaskelainen A., Hartikainen A.L., Sovio U., Vaarasmaki M., Pouta A., Kaakinen M., Jarvelin M.R. Maternal weight gain during the first half of pregnancy and offspring obesity at 16 years: A prospective cohort study. BJOG. 2012;119:716–723. doi: 10.1111/j.1471-0528.2012.03319.x. - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

