Aggressive or moderate drug therapy for infectious diseases? Trade-offs between different treatment goals at the individual and population levels
- PMID: 31404059
- PMCID: PMC6742410
- DOI: 10.1371/journal.pcbi.1007223
Aggressive or moderate drug therapy for infectious diseases? Trade-offs between different treatment goals at the individual and population levels
Abstract
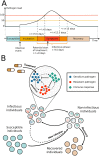
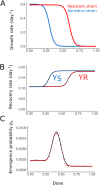
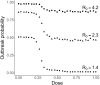
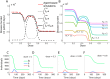
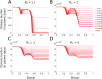
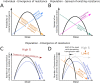
Antimicrobial resistance is one of the major public health threats of the 21st century. There is a pressing need to adopt more efficient treatment strategies in order to prevent the emergence and spread of resistant strains. The common approach is to treat patients with high drug doses, both to clear the infection quickly and to reduce the risk of de novo resistance. Recently, several studies have argued that, at least in some cases, low-dose treatments could be more suitable to reduce the within-host emergence of antimicrobial resistance. However, the choice of a drug dose may have consequences at the population level, which has received little attention so far. Here, we study the influence of the drug dose on resistance and disease management at the host and population levels. We develop a nested two-strain model and unravel trade-offs in treatment benefits between an individual and the community. We use several measures to evaluate the benefits of any dose choice. Two measures focus on the emergence of resistance, at the host level and at the population level. The other two focus on the overall treatment success: the outbreak probability and the disease burden. We find that different measures can suggest different dosing strategies. In particular, we identify situations where low doses minimize the risk of emergence of resistance at the individual level, while high or intermediate doses prove most beneficial to improve the treatment efficiency or even to reduce the risk of resistance in the population.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


References
-
- Boucher HW, Talbot GH, Bradley JS, Edwards JE, Gilbert D, Rice LB, et al. Bad bugs, no drugs: no ESKAPE! An update from the Infectious Diseases Society of America. Clinical infectious diseases: an official publication of the Infectious Diseases Society of America. 2009;48(1):1–12. 10.1086/595011 - DOI - PubMed
-
- Centres for Disease Control and Prevention (US). Antibiotic resistance threats in the United States, 2013. Centres for Disease Control and Prevention, US Department of Health and Human Services; 2013.
-
- O’Neill J. Tackling drug-resistant infections globally: final report and recommendations. Review on Antimicrobial Resistance. 2016;.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

