Association of Thyroid Function Test Abnormalities and Thyroid Autoimmunity With Preterm Birth: A Systematic Review and Meta-analysis
- PMID: 31429897
- PMCID: PMC6704759
- DOI: 10.1001/jama.2019.10931
Association of Thyroid Function Test Abnormalities and Thyroid Autoimmunity With Preterm Birth: A Systematic Review and Meta-analysis
Erratum in
-
Incorrect Spelling of Author Name, Incorrect Affiliation of Another Author, and Removal of Academic Degree.JAMA. 2019 Nov 5;322(17):1718. doi: 10.1001/jama.2019.16269. JAMA. 2019. PMID: 31688866 No abstract available.
Abstract
Importance: Maternal hypothyroidism and hyperthyroidism are risk factors for preterm birth. Milder thyroid function test abnormalities and thyroid autoimmunity are more prevalent, but it remains controversial if these are associated with preterm birth.
Objective: To study if maternal thyroid function test abnormalities and thyroid autoimmunity are risk factors for preterm birth.
Data sources and study selection: Studies were identified through a search of the Ovid MEDLINE, EMBASE, Web of Science, the Cochrane Central Register of Controlled Trials, and Google Scholar databases from inception to March 18, 2018, and by publishing open invitations in relevant journals. Data sets from published and unpublished prospective cohort studies with data on thyroid function tests (thyrotropin [often referred to as thyroid-stimulating hormone or TSH] and free thyroxine [FT4] concentrations) or thyroid peroxidase (TPO) antibody measurements and gestational age at birth were screened for eligibility by 2 independent reviewers. Studies in which participants received treatment based on abnormal thyroid function tests were excluded.
Data extraction and synthesis: The primary authors provided individual participant data that were analyzed using mixed-effects models.
Main outcomes and measures: The primary outcome was preterm birth (<37 weeks' gestational age).
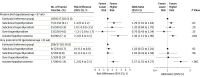
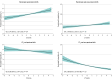
Results: From 2526 published reports, 35 cohorts were invited to participate. After the addition of 5 unpublished data sets, a total of 19 cohorts were included. The study population included 47 045 pregnant women (mean age, 29 years; median gestational age at blood sampling, 12.9 weeks), of whom 1234 (3.1%) had subclinical hypothyroidism (increased thyrotropin concentration with normal FT4 concentration), 904 (2.2%) had isolated hypothyroxinemia (decreased FT4 concentration with normal thyrotropin concentration), and 3043 (7.5%) were TPO antibody positive; 2357 (5.0%) had a preterm birth. The risk of preterm birth was higher for women with subclinical hypothyroidism than euthyroid women (6.1% vs 5.0%, respectively; absolute risk difference, 1.4% [95% CI, 0%-3.2%]; odds ratio [OR], 1.29 [95% CI, 1.01-1.64]). Among women with isolated hypothyroxinemia, the risk of preterm birth was 7.1% vs 5.0% in euthyroid women (absolute risk difference, 2.3% [95% CI, 0.6%-4.5%]; OR, 1.46 [95% CI, 1.12-1.90]). In continuous analyses, each 1-SD higher maternal thyrotropin concentration was associated with a higher risk of preterm birth (absolute risk difference, 0.2% [95% CI, 0%-0.4%] per 1 SD; OR, 1.04 [95% CI, 1.00-1.09] per 1 SD). Thyroid peroxidase antibody-positive women had a higher risk of preterm birth vs TPO antibody-negative women (6.6% vs 4.9%, respectively; absolute risk difference, 1.6% [95% CI, 0.7%-2.8%]; OR, 1.33 [95% CI, 1.15-1.56]).
Conclusions and relevance: Among pregnant women without overt thyroid disease, subclinical hypothyroidism, isolated hypothyroxinemia, and TPO antibody positivity were significantly associated with higher risk of preterm birth. These results provide insights toward optimizing clinical decision-making strategies that should consider the potential harms and benefits of screening programs and levothyroxine treatment during pregnancy.
Conflict of interest statement
Figures


Comment in
-
Thyroid Function Test Abnormalities During Pregnancy.JAMA. 2019 Aug 20;322(7):617-619. doi: 10.1001/jama.2019.10159. JAMA. 2019. PMID: 31429879 No abstract available.
References
-
- Blencowe H, Cousens S, Oestergaard MZ, et al. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet. 2012;379(9832):2162-2172. doi: 10.1016/S0140-6736(12)60820-4 - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

