Comparison of nonlinear microscopy and frozen section histology for imaging of Mohs surgical margins
- PMID: 31453008
- PMCID: PMC6701533
- DOI: 10.1364/BOE.10.004249
Comparison of nonlinear microscopy and frozen section histology for imaging of Mohs surgical margins
Abstract
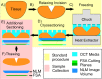
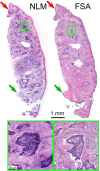
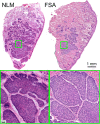
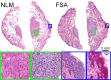
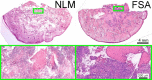
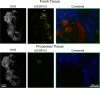
Mohs surgery uses en face frozen section analysis (FSA) with complete margin examination for the excision of select basal cell carcinomas (BCC), obtaining excellent cosmetic outcomes and extremely low recurrence rates. However, Mohs with FSA is time-consuming because of the need to iteratively perform cryosectioning on sequential excisions. Fluorescent microscopies can image tissue specimens without requiring physical sectioning, potentially reducing the time to perform Mohs surgery. We demonstrate a protocol for nonlinear microscopy (NLM) imaging of surgical specimens that combines dual agent staining, virtual H&E rendering, and video rate imaging. We also introduce a novel protocol that enables micron-level co-registration of NLM images with FSA histology, and demonstrate that NLM can reproduce similar features similar to FSA in BCC specimens with both negative and positive surgical margins. We show that the fluorescent labels can be extracted with conventional vacuum infiltration processing, enabling subsequent immunohistochemistry on fluorescently labeled tissue. This protocol can also be applied to evaluate the performance of NLM compared with FSA in a wide range of pathologies for intraoperative consultation.
Conflict of interest statement
The authors declare that there are no conflicts of interest related to this article.
Figures


Similar articles
-
Multiscale nonlinear microscopy and widefield white light imaging enables rapid histological imaging of surgical specimen margins.Biomed Opt Express. 2018 Apr 30;9(5):2457-2475. doi: 10.1364/BOE.9.002457. eCollection 2018 May 1. Biomed Opt Express. 2018. PMID: 29761001 Free PMC article.
-
A comparison of touch imprint cytology and Mohs frozen-section histology in the evaluation of Mohs micrographic surgical margins.J Am Acad Dermatol. 2001 Apr;44(4):660-4. doi: 10.1067/mjd.2001.112216. J Am Acad Dermatol. 2001. PMID: 11260543
-
Assessment of breast pathologies using nonlinear microscopy.Proc Natl Acad Sci U S A. 2014 Oct 28;111(43):15304-9. doi: 10.1073/pnas.1416955111. Epub 2014 Oct 13. Proc Natl Acad Sci U S A. 2014. PMID: 25313045 Free PMC article.
-
Is frozen section analysis of ureteral margins at time of radical cystectomy useful?Curr Urol Rep. 2015 Jun;16(6):38. doi: 10.1007/s11934-015-0506-x. Curr Urol Rep. 2015. PMID: 25940187 Review.
-
Role of In Vivo Reflectance Confocal Microscopy in the Analysis of Melanocytic Lesions.Acta Dermatovenerol Croat. 2018 Apr;26(1):64-67. Acta Dermatovenerol Croat. 2018. PMID: 29782304 Review.
Cited by
-
Improved microscopy with ultraviolet surface excitation (MUSE) using high-index immersion illumination.Biomed Opt Express. 2021 Sep 22;12(10):6461-6473. doi: 10.1364/BOE.435520. eCollection 2021 Oct 1. Biomed Opt Express. 2021. PMID: 34745749 Free PMC article.
-
High-speed mosaic imaging using scanner-synchronized stage position sampling.J Biomed Opt. 2022 Jan;27(1):016502. doi: 10.1117/1.JBO.27.1.016502. J Biomed Opt. 2022. PMID: 35075830 Free PMC article.
-
Rapid examination of lung tissues by nonlinear microscopy.Am J Clin Pathol. 2024 Oct 3;162(4):369-378. doi: 10.1093/ajcp/aqae046. Am J Clin Pathol. 2024. PMID: 38682548 Free PMC article.
-
Fast, large area multiphoton exoscope (FLAME) for macroscopic imaging with microscopic resolution of human skin.Sci Rep. 2020 Oct 22;10(1):18093. doi: 10.1038/s41598-020-75172-9. Sci Rep. 2020. PMID: 33093610 Free PMC article.
-
Rapid Examination of Nonprocessed Renal Cell Carcinoma Using Nonlinear Microscopy.Arch Pathol Lab Med. 2024 Dec 1;148(12):1320-1326. doi: 10.5858/arpa.2023-0320-OA. Arch Pathol Lab Med. 2024. PMID: 38411182
References
-
- American Cancer Society, “Cancer Facts & Figures 2018,” http://www.cancer.org/research/cancerfactsstatistics/cancerfactsfigures2....
-
- Tierney E. P., Hanke C. W., “Cost effectiveness of Mohs micrographic surgery: review of the literature,” J. Drugs Dermatol. 8(10), 914–922 (2009). - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
