Comparison of NIV-NAVA and NCPAP in facilitating extubation for very preterm infants
- PMID: 31462232
- PMCID: PMC6712684
- DOI: 10.1186/s12887-019-1683-4
Comparison of NIV-NAVA and NCPAP in facilitating extubation for very preterm infants
Abstract
Background: Various types of noninvasive respiratory modalities that lead to successful extubation in preterm infants have been explored. We aimed to compare noninvasive neurally adjusted ventilatory assist (NIV-NAVA) and nasal continuous positive airway pressure (NCPAP) for the postextubation stabilization of preterm infants.
Methods: This retrospective study was divided into two distinct periods, between July 2012 and June 2013 and between July 2013 and June 2014, because NIV-NAVA was applied beginning in July 2013. Preterm infants of less than 30 weeks GA who had been intubated with mechanical ventilation for longer than 24 h and were weaned to NCPAP or NIV-NAVA after extubation were enrolled. Ventilatory variables and extubation failure were compared after weaning to NCPAP or NIV-NAVA. Extubation failure was defined when infants were reintubated within 72 h of extubation.
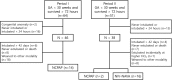
Results: There were 14 infants who were weaned to NCPAP during Period I, and 2 infants and 16 infants were weaned to NCPAP and NIV-NAVA, respectively, during Period II. At the time of extubation, there were no differences in the respiratory severity score (NIV-NAVA 1.65 vs. NCPAP 1.95), oxygen saturation index (1.70 vs. 2.09) and steroid use before extubation. Several ventilation parameters at extubation, such as the mean airway pressure, positive end-expiratory pressure, peak inspiratory pressure, and FiO2, were similar between the two groups. SpO2 and pCO2 preceding extubation were comparable. Extubation failure within 72 h after extubation was observed in 6.3% of the NIV-NAVA group and 37.5% of the NCPAP group (P = 0.041).
Conclusions: The data in the present showed promising implications for using NIV-NAVA over NCPAP to facilitate extubation.
Keywords: Airway extubation; Continuous positive airway pressure; Neurally adjusted ventilator assist; Noninvasive ventilation; Ventilator weaning.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
-
- Moretti C, Giannini L, Fassi C, Gizzi C, Papoff P, Colarizi P. Nasal flow-synchronized intermittent positive pressure ventilation to facilitate weaning in very low-birthweight infants: unmasked randomized controlled trial. Pediatr Int. 2008;50(1):85–91. doi: 10.1111/j.1442-200X.2007.02525.x. - DOI - PubMed
-
- Khalaf MN, Brodsky N, Hurley J, Bhandari V. A prospective randomized, controlled trial comparing synchronized nasal intermittent positive pressure ventilation versus nasal continuous positive airway pressure as modes of extubation. Pediatrics. 2001;108(1):13–17. doi: 10.1542/peds.108.1.13. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources