Implementing eScreening technology in four VA clinics: a mixed-method study
- PMID: 31462280
- PMCID: PMC6712612
- DOI: 10.1186/s12913-019-4436-z
Implementing eScreening technology in four VA clinics: a mixed-method study
Abstract
Background: Technology-based self-assessment (TB-SA) benefits patients and providers and has shown feasibility, ease of use, efficiency, and cost savings. A promising TB-SA, the VA eScreening program, has shown promise for the efficient and effective collection of mental and physical health information. To assist adoption of eScreening by healthcare providers, we assessed technology-related as well as individual- and system-level factors that might influence the implementation of eScreening in four diverse VA clinics.
Methods: This was a mixed-method, pre-post, quasi-experimental study originally designed as a quality improvement project. The clinics were selected to represent a range of environments that could potentially benefit from TB-SA and that made use of the variety eScreening functions. Because of limited resources, the implementation strategy consisted of staff education, training, and technical support as needed. Data was collected using pre- and post-implementation interviews or focus groups of leadership and clinical staff, eScreening usage data, and post-implementation surveys. Data was gathered on: 1) usability of eScreening; 2) knowledge about and acceptability and 3) facilitators and barriers to the successful implementation of eScreening.
Results: Overall, staff feedback about eScreening was positive. Knowledge about eScreening ranged widely between the clinics. Nearly all staff felt eScreening would fit well into their clinical setting at pre-implementation; however some felt it was a poor fit with emergent cases and older adults at post-implementation. Lack of adequate personnel support and perceived leadership support were barriers to implementation. Adequate training and technical assistance were cited as important facilitators. One clinic fully implemented eScreening, two partially implemented, and one clinic did not implement eScreening as part of normal practice after 6 months as measured by usage data and self-report. Organizational engagement survey scores were higher among clinics with full or partial implementation and low in the clinic that did not implement.
Conclusions: Despite some added work load for some staff and perceived lack of leadership support, eScreening was at least partially implemented in three clinics. The technology itself posed no barriers in any of the settings. An implementation strategy that accounts for increased work burden and includes accountability may help in future eScreening implementation efforts. Note. This abstract was previously published (e.g., Annals of Behavioral Medicine 53: S1-S842, 2019).
Keywords: Health information technology; Implementation; Mixed methods; Technology; Veterans; eScreening.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
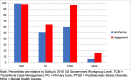
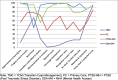
References
-
- Shekelle P, Morton S, Keeler E. Costs and benefits of health information technology. Evidence report/technology assessment no. 132. (prepared by the Southern California evidence-based practice center under contract no. 290–02-0003.) AHRQ publication no. 06-E006. Rockville, MD: Agency for Healthcare Research and Quality. April 2006.
-
- Aktas Aynur, Hullihen Barbara, Shrotriya Shiva, Thomas Shirley, Walsh Declan, Estfan Bassam. Connected Health: Cancer Symptom and Quality-of-Life Assessment Using a Tablet Computer. American Journal of Hospice and Palliative Medicine®. 2013;32(2):189–197. - PubMed
-
- Hjermstad M, Lie H, Caraceni A, Currow D, Fainsinger R, Gundersen O, et al. Computer-based symptom assessment is feasible in patients with advanced Cancer: results from an international multicenter study, the EPCRC-CSA. J Pain Symptom Manag. 2012;44(5):639–654. - PubMed

