Predicting developmental outcomes in preterm infants: A simple white matter injury imaging rule
- PMID: 31467250
- PMCID: PMC7011867
- DOI: 10.1212/WNL.0000000000008172
Predicting developmental outcomes in preterm infants: A simple white matter injury imaging rule
Abstract
Objective: To develop a simple imaging rule to predict neurodevelopmental outcomes at 4.5 years in a cohort of preterm neonates with white matter injury (WMI) based on lesion location and examine whether clinical variables enhance prediction.
Methods: Sixty-eight preterm neonates born 24-32 weeks' gestation (median 27.7 weeks) were diagnosed with WMI on early brain MRI scans (median 32.3 weeks). 3D T1-weighted images of 60 neonates with 4.5-year outcomes were reformatted and aligned to the posterior commissure-eye plane and WMI was classified by location: anterior or posterior-only to the midventricle line on the reformatted axial plane. Adverse outcomes at 4.5 years were defined as Wechsler Preschool and Primary Scale of Intelligence full-scale IQ <85, cerebral palsy, or Movement Assessment Battery for Children, second edition percentile <5. The prediction of adverse outcome by WMI location, intraventricular hemorrhage (IVH), bronchopulmonary dysplasia (BPD), and retinopathy of prematurity (ROP) was assessed using multivariable logistic regression.
Results: Six children had adverse cognitive outcomes and 17 had adverse motor outcomes. WMI location predicted cognitive outcomes in 90% (area under receiver operating characteristic curve [AUC] 0.80) and motor outcomes in 85% (AUC 0.75). Adding IVH, BPD, and ROP to the model enhances the predictive strength for cognitive and motor outcomes (AUC 0.83 and 0.88, respectively). Rule performance was confirmed in an independent cohort of children with WMI.
Conclusions: WMI on early MRI can be classified by location to predict preschool age outcomes in children born preterm. The predictive value of this WMI classification is enhanced by considering clinical factors apparent by term-equivalent age.
© 2019 American Academy of Neurology.
Figures

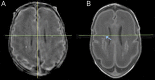
Comment in
-
When white matter lesions cross the (midventricle) line: Predicting outcome in preterm infants.Neurology. 2019 Sep 24;93(13):569-570. doi: 10.1212/WNL.0000000000008165. Epub 2019 Aug 29. Neurology. 2019. PMID: 31467254 No abstract available.
References
-
- Dyet LE, Kennea N, Counsell SJ, et al. Natural history of brain lesions in extremely preterm infants studied with serial magnetic resonance imaging from birth and neurodevelopmental assessment. Pediatrics 2006;118:536–548. - PubMed
-
- Volpe JJ. Cerebral white matter injury of the premature infant: more common than you think. Pediatrics 2003;112:176–180. - PubMed
-
- Back SA. Perinatal white matter injury: the changing spectrum of pathology and emerging insights into pathogenetic mechanisms. Ment Retard Dev Disabil Res Rev 2006;12:129–140. - PubMed
