Comparison of High Doses of Total Body Irradiation in Myeloablative Conditioning before Hematopoietic Cell Transplantation
- PMID: 31473319
- PMCID: PMC7304318
- DOI: 10.1016/j.bbmt.2019.08.012
Comparison of High Doses of Total Body Irradiation in Myeloablative Conditioning before Hematopoietic Cell Transplantation
Abstract
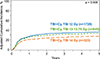
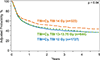
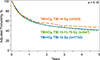
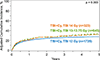
Malignancy relapse is the most common cause of treatment failure among recipients of hematopoietic cell transplantation (HCT). Conditioning dose intensity can reduce disease relapse but is offset by toxicities. Improvements in radiotherapy techniques and supportive care may translate to better outcomes with higher irradiation doses in the modern era. This study compares outcomes of recipients of increasing doses of high-dose total body irradiation (TBI) divided into intermediate high dose (IH; 13-13.75 Gy) and high dose (HD; 14 Gy) with standard dose (SD; 12 Gy) with cyclophosphamide. A total of 2721 patients ages 18 to 60 years with hematologic malignancies receiving HCT from 2001 to 2013 were included. Cumulative incidences of nonrelapse mortality (NRM) at 5 years were 28% (95% confidence interval [CI], 25% to 30%), 32% (95% CI, 29% to 36%), and 34% (95% CI, 28% to 39%) for SD, IH, and HD, respectively (P = .02). Patients receiving IH-TBI had a 25% higher risk of NRM compared with those receiving SD-TBI (12 Gy) (P = .007). Corresponding cumulative incidences of relapse were 36% (95% CI, 34% to 38%), 32% (95% CI, 29% to 36%), and 26% (95% CI, 21% to 31%; P = .001). Hazard ratios for mortality compared with SD were 1.06 (95% CI, .94 to 1.19; P = .36) for IH and .89 (95% CI, .76 to 1.05; P = .17) for HD. The study demonstrates that despite improvements in supportive care, myeloablative conditioning using higher doses of TBI (with cyclophosphamide) leads to worse NRM and offers no survival benefit over SD, despite reducing disease relapse.
Keywords: Allogeneic hematopoietic cell transplantation; Hematologic malignancies; Myeloablative conditioning; Total body irradiation.
Copyright © 2019 American Society for Transplantation and Cellular Therapy. Published by Elsevier Inc. All rights reserved.
Figures
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources