Prescription Drug Monitoring Program Mandates: Impact On Opioid Prescribing And Related Hospital Use
- PMID: 31479368
- PMCID: PMC6824582
- DOI: 10.1377/hlthaff.2019.00103
Prescription Drug Monitoring Program Mandates: Impact On Opioid Prescribing And Related Hospital Use
Abstract
Comprehensive mandates for prescription drug monitoring programs (PDMPs) require state-licensed prescribers and dispensers both to register with and to use the programs in most clinical circumstances. Such mandates have the potential to improve providers' participation and reduce opioid-related adverse events. Using Medicaid prescription data and hospital utilization data across the US in the period 2011-16, we found that state implementation of comprehensive PDMP mandates was associated with a reduction in the opioid prescription rate from 161.47 to 147.07 per 1,000 enrollees per quarter, a reduction in the opioid-related inpatient stay rate from 97.50 to 93.34 per 100,000 enrollees per quarter, and a reduction in the opioid-related emergency department (ED) visit rate from 74.60 to 61.36 per 100,000 enrollees per quarter. Our estimated annual reductions of approximately 12,000 inpatient stays and 39,000 ED visits could save over $155 million in Medicaid spending, a fact that deserves policy attention when states attempt to strengthen and refine PDMPs to better tackle the opioid crisis.
Figures

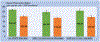
References
-
- Council of Economic Advisers (CEA), Executive Office of the President of the United States. The underestimated cost of the opioid crisis [Internet]. Washington, DC: The White House; 2017. November 19 [cited 2019 Apr 25]. https://www.whitehouse.gov/sites/whitehouse.gov/files/images/The%20Under...
-
- Bohnert AS, Valenstein M, Bair MJ, Ganoczy D, McCarthy JF, Ilgen MA, et al. Association between opioid prescribing patterns and opioid overdose-related deaths. JAMA. 2011. April 6;305(13):1315–21. - PubMed
-
- Madras BK. The surge of opioid use, addiction, and overdoses: responsibility and response of the US health care system. JAMA Psychiatry. 2017. May 1;74(5):441–2. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

