Chronic white matter lesion activity predicts clinical progression in primary progressive multiple sclerosis
- PMID: 31497864
- PMCID: PMC6736181
- DOI: 10.1093/brain/awz212
Chronic white matter lesion activity predicts clinical progression in primary progressive multiple sclerosis
Abstract
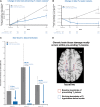
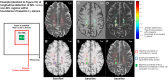
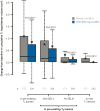
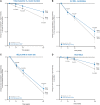
Chronic active and slowly expanding lesions with smouldering inflammation are neuropathological correlates of progressive multiple sclerosis pathology. T1 hypointense volume and signal intensity on T1-weighted MRI reflect brain tissue damage that may develop within newly formed acute focal inflammatory lesions or in chronic pre-existing lesions without signs of acute inflammation. Using a recently developed method to identify slowly expanding/evolving lesions in vivo from longitudinal conventional T2- and T1-weighted brain MRI scans, we measured the relative amount of chronic lesion activity as measured by change in T1 volume and intensity within slowly expanding/evolving lesions and non-slowly expanding/evolving lesion areas of baseline pre-existing T2 lesions, and assessed the effect of ocrelizumab on this outcome in patients with primary progressive multiple sclerosis participating in the phase III, randomized, placebo-controlled, double-blind ORATORIO study (n = 732, NCT01194570). We also assessed the predictive value of T1-weighted measures of chronic lesion activity for clinical multiple sclerosis progression as reflected by a composite disability measure including the Expanded Disability Status Scale, Timed 25-Foot Walk and 9-Hole Peg Test. We observed in this clinical trial population that most of total brain non-enhancing T1 hypointense lesion volume accumulation was derived from chronic lesion activity within pre-existing T2 lesions rather than new T2 lesion formation. There was a larger decrease in mean normalized T1 signal intensity and greater relative accumulation of T1 hypointense volume in slowly expanding/evolving lesions compared with non-slowly expanding/evolving lesions. Chronic white matter lesion activity measured by longitudinal T1 hypointense lesion volume accumulation in slowly expanding/evolving lesions and in non-slowly expanding/evolving lesion areas of pre-existing lesions predicted subsequent composite disability progression with consistent trends on all components of the composite. In contrast, whole brain volume loss and acute lesion activity measured by longitudinal T1 hypointense lesion volume accumulation in new focal T2 lesions did not predict subsequent composite disability progression in this trial at the population level. Ocrelizumab reduced longitudinal measures of chronic lesion activity such as T1 hypointense lesion volume accumulation and mean normalized T1 signal intensity decrease both within regions of pre-existing T2 lesions identified as slowly expanding/evolving and in non-slowly expanding/evolving lesions. Using conventional brain MRI, T1-weighted intensity-based measures of chronic white matter lesion activity predict clinical progression in primary progressive multiple sclerosis and may qualify as a longitudinal in vivo neuroimaging correlate of smouldering demyelination and axonal loss in chronic active lesions due to CNS-resident inflammation and/or secondary neurodegeneration across the multiple sclerosis disease continuum.
Keywords: MS: biomarkers; MS: clinical trials; MS: imaging; neuroinflammation; white matter lesion.
© The Author(s) (2019). Published by Oxford University Press on behalf of the Guarantors of Brain.
Figures
Comment in
-
Early MRI predictors of prognosis in multiple sclerosis.J Neurol. 2019 Dec;266(12):3171-3173. doi: 10.1007/s00415-019-09589-2. J Neurol. 2019. PMID: 31701334 Free PMC article. No abstract available.
References
-
- Bosma LV, Kragt JJ, Brieva L, Khaleeli Z, Montalban X, Polman CH et al. The search for responsive clinical endpoints in primary progressive multiple sclerosis. Mult Scler J 2009; 15: 715–20. - PubMed
-
- Bramow S, Frischer JM, Lassmann H, Koch-Henriksen N, Lucchinetti CF, Sørensen PS. Demyelination versus remyelination in progressive multiple sclerosis. Brain 2010; 133: 2983–98. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

