Structure and severity of pharyngeal obstruction determine oral appliance efficacy in sleep apnoea
- PMID: 31503323
- PMCID: PMC8359733
- DOI: 10.1113/JP278164
Structure and severity of pharyngeal obstruction determine oral appliance efficacy in sleep apnoea
Abstract
Key points: •Some patients with obstructive sleep apnoea (OSA) respond well to oral appliance therapy, whereas others do not for reasons that are unclear. •In the present study, we used gold-standard measurements to demonstrate that patients with a posteriorly-located tongue (natural sleep endoscopy) exhibit a preferential improvement in collapsibility (lowered critical closing pressure) with oral appliances. •We also show that patients with both posteriorly-located tongue and less severe collapsibility (predicted responder phenotype) exhibit greater improvements in severity of obstructive sleep apnoea (i.e. reduction in event frequency by 83%, in contrast to 48% in predicted non-responders). •The present study suggests that the structure and severity of pharyngeal obstruction determine the phenotype of sleep apnoea patients who benefit maximally from oral appliance efficacy.
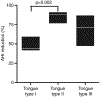
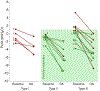
Abstract: A major limitation to the administration of oral appliance therapy for obstructive sleep apnoea (OSA) is that therapeutic responses remain unpredictable. In the present study, we tested the hypotheses that oral appliance therapy (i) reduces pharyngeal collapsibility preferentially in patients with posteriorly-located tongue and (ii) is most efficacious (reduction in apnoea-hypopnea index; AHI) in patients with a posteriorly-located tongue and less-severe baseline pharyngeal collapsibility. Twenty-five OSA patients underwent upper airway endoscopy during natural sleep to assess tongue position (type I: vallecula entirely visible; type II: vallecula obscured; type III: vallecula and glottis obscured), as well as obstruction as a result of other pharyngeal structures (e.g. epiglottis). Additional sleep studies with and without oral appliance were performed to measure collapsibility (critical closing pressure; Pcrit) and assess treatment efficacy. Overall, oral appliance therapy reduced Pcrit by 3.9 ± 2.4 cmH2 O (mean ± SD) and AHI by 69 ± 19%. Therapy lowered Pcrit by an additional 2.7 ± 0.9 cmH2 O in patients with posteriorly-located tongue (types II and III) compared to those without (type I) (P < 0.008). Posteriorly-located tongue (p = 0.03) and lower collapsibility (p = 0.04) at baseline were significant determinants of (greater-than-average) treatment efficacy. Predicted responders (type II and III and Pcrit < 1 cmH2 O) exhibited a greater reduction in the AHI (83 ± 9 vs. 48 ± 8% baseline, P < 0.001) and a lower treatment AHI (9 ± 6 vs. 32 ± 15 events h-1 , P < 0.001) than predicted non-responders. The site and severity of pharyngeal collapse combine to determine oral appliance efficacy. Specifically, patients with a posteriorly-located tongue plus less-severe collapsibility are the strongest candidates for oral appliance therapy.
© 2019 The Authors. The Journal of Physiology © 2019 The Physiological Society.
Figures

Comment in
-
Moving beyond an empiric trial to using combined physiology and anatomy to predict success of oral appliances in obstructive sleep apnoea.J Physiol. 2019 Nov;597(22):5321. doi: 10.1113/JP278922. Epub 2019 Oct 30. J Physiol. 2019. PMID: 31549391 No abstract available.
Similar articles
-
Response to a combination of oxygen and a hypnotic as treatment for obstructive sleep apnoea is predicted by a patient's therapeutic CPAP requirement.Respirology. 2017 Aug;22(6):1219-1224. doi: 10.1111/resp.13044. Epub 2017 Apr 13. Respirology. 2017. PMID: 28409851 Free PMC article. Clinical Trial.
-
Polysomnographic Endotyping to Select Patients with Obstructive Sleep Apnea for Oral Appliances.Ann Am Thorac Soc. 2019 Nov;16(11):1422-1431. doi: 10.1513/AnnalsATS.201903-190OC. Ann Am Thorac Soc. 2019. PMID: 31394914 Free PMC article. Clinical Trial.
-
Dose-dependent effects of mandibular advancement on upper airway collapsibility and muscle function in obstructive sleep apnea.Sleep. 2019 Jun 11;42(6):zsz049. doi: 10.1093/sleep/zsz049. Sleep. 2019. PMID: 30810164
-
Anatomical determinants of upper airway collapsibility in obstructive sleep apnea: A systematic review and meta-analysis.Sleep Med Rev. 2023 Apr;68:101741. doi: 10.1016/j.smrv.2022.101741. Epub 2022 Dec 30. Sleep Med Rev. 2023. PMID: 36634409 Free PMC article.
-
Appliances Therapy in Obstructive Sleep Apnoea: A Systematic Review and Meta-Analysis.Cureus. 2023 Nov 4;15(11):e48280. doi: 10.7759/cureus.48280. eCollection 2023 Nov. Cureus. 2023. PMID: 38058324 Free PMC article. Review.
Cited by
-
In-home mandibular repositioning during sleep using MATRx plus predicts outcome and efficacious positioning for oral appliance treatment of obstructive sleep apnea.J Clin Sleep Med. 2022 Mar 1;18(3):911-919. doi: 10.5664/jcsm.9758. J Clin Sleep Med. 2022. PMID: 34747691 Free PMC article.
-
Is Obstructive Sleep Apnea in People Without Obesity a Unique Disease?Arch Bronconeumol. 2025 Jul;61(7):393-394. doi: 10.1016/j.arbres.2025.02.014. Epub 2025 Mar 1. Arch Bronconeumol. 2025. PMID: 40118688 No abstract available.
-
Mandibular Advancement Device Treatment Efficacy Is Associated with Polysomnographic Endotypes.Ann Am Thorac Soc. 2021 Mar;18(3):511-518. doi: 10.1513/AnnalsATS.202003-220OC. Ann Am Thorac Soc. 2021. PMID: 32946702 Free PMC article. Clinical Trial.
-
Clinical polysomnographic methods for estimating pharyngeal collapsibility in obstructive sleep apnea.Sleep. 2022 Jun 13;45(6):zsac050. doi: 10.1093/sleep/zsac050. Sleep. 2022. PMID: 35238379 Free PMC article.
-
Non-CPAP therapy for obstructive sleep apnoea.Breathe (Sheff). 2022 Sep;18(3):220164. doi: 10.1183/20734735.0164-2022. Epub 2022 Oct 11. Breathe (Sheff). 2022. PMID: 36340820 Free PMC article. Review.
References
-
- Azarbarzin A, Sands SA, Marques M, Genta PR, Taranto-Montemurro L, Messineo L, White DP & Wellman A (2018). Palatal prolapse as a signature of expiratory flow limitation and inspiratory palatal collapse in patients with obstructive sleep apnoea. Eur Respir J 51, 1701419. 10.1183/13993003.01419-2017. - DOI - PMC - PubMed
-
- Bamagoos AA, Cistulli P, Sutherland K, Ngiam J, Burke P, Bilston L, Butler JE & Eckert DJ (2017). Dose-dependent effects of mandibular advancement on upper airway collapsibility and muscle activity in obstructive sleep apnea. Am J Respir Crit Care Med 195, A6972. - PubMed
-
- Bamagoos AA, Sutherland K & Cistulli PA (2016). Mandibular advancement splints. Sleep Med Clin 11, 343–352. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

