Dietary intakes of flavan-3-ols and cardiometabolic health: systematic review and meta-analysis of randomized trials and prospective cohort studies
- PMID: 31504087
- PMCID: PMC6821550
- DOI: 10.1093/ajcn/nqz178
Dietary intakes of flavan-3-ols and cardiometabolic health: systematic review and meta-analysis of randomized trials and prospective cohort studies
Abstract
Background: Although available data suggest that some dietary flavan-3-ol sources reduce cardiometabolic risk, to our knowledge no review has systematically synthesized their specific contribution.
Objective: We aimed to examine, for the first time, if there is consistent evidence that higher flavan-3-ol intake, irrespective of dietary source, reduces cardiometabolic risk.
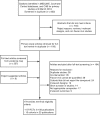
Methods: MEDLINE, Cochrane Central, and Commonwealth Agricultural Bureau abstracts were searched for prospective cohorts and randomized controlled trials (RCTs) published from 1946 to March 2019 on flavan-3-ol intake and cardiovascular disease (CVD) risk. Random-effects models meta-analysis was used. The Grading of Recommendations Assessment, Development, and Evaluation (GRADE) approach assessed the strength of evidence.
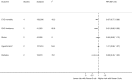
Results: Of 15 prospective cohorts (23 publications), 4 found highest compared with lowest habitual intakes of flavan-3-ols were associated with a 13% reduction in risk of CVD mortality and 2 found a 19% reduction in risk of chronic heart disease (CHD) incidence. Highest compared with lowest habitual intakes of monomers were associated with a reduction in risk of type 2 diabetes mellitus (T2DM) (n = 5) and stroke (n = 4) (10% and 18%, respectively). No association was found for hypertension. Of 156 RCTs, flavan-3-ol intervention resulted in significant improvements in acute/chronic flow-mediated dilation (FMD), systolic (SBP) and diastolic blood pressure (DBP), total cholesterol (TC), LDL and HDL cholesterol, triglycerides (TGs), hemoglobin A1c (HbA1c), and homeostasis model assessment of insulin resistance (HOMA-IR). All analyses, except HbA1c, were associated with moderate/high heterogeneity. When analyses were limited to good methodological quality studies, improvements in TC, HDL cholesterol, SBP, DBP, HOMA-IR, and acute/chronic FMD remained significant. In GRADE evaluations, there was moderate evidence in cohort studies that flavan-3-ol and monomer intakes were associated with reduced risk of CVD mortality, CHD, stroke, and T2DM, whereas RCTs reported improved TC, HDL cholesterol, SBP, and HOMA-IR.
Conclusions: Available evidence supports a beneficial effect of flavan-3-ol intake on cardiometabolic outcomes, but there was considerable heterogeneity in the meta-analysis. Future research should focus on an integrated intake/biomarker approach in cohorts and high-quality dose-response RCTs. This review was registered at www.crd.york.ac.uk/PROSPERO/ as CRD42018035782.
Keywords: blood pressure; cardiovascular; diabetes; flavan-3-ols; flavonoids.
Copyright © American Society for Nutrition 2019.
Figures

References
-
- Perez-Vizcaino F, Fraga CG. Research trends in flavonoids and health. Arch Biochem Biophys. 2018;646:107–12. - PubMed
-
- Rodriguez-Mateos A, Vauzour D, Krueger CG, Shanmuganayagam D, Reed J, Calani L, Mena P, Del Rio D, Crozier A. Bioavailability, bioactivity and impact on health of dietary flavonoids and related compounds: an update. Arch Toxicol. 2014;88:1803–53. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

