Sarcopenia does not affect postoperative complication rates in oesophageal cancer surgery: a systematic review and meta-analysis
- PMID: 31508983
- PMCID: PMC6996429
- DOI: 10.1308/rcsann.2019.0113
Sarcopenia does not affect postoperative complication rates in oesophageal cancer surgery: a systematic review and meta-analysis
Abstract
Introduction: The high morbidity and mortality rates after oesophagectomy indicate the need for rigorous patient selection and preoperative risk assessment. Although muscle mass depletion has been proposed as a potential prognostic factor for postoperative complications and decreased survival in gastrointestinal cancer patients, available data are conflicting. The purpose of the present meta-analysis is to determine whether sarcopenia predicts postoperative outcomes in patients undergoing oesophagectomy.
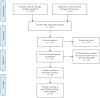
Methods: The databases MEDLINE, SCOPUS, Clinicaltrials.gov, CENTRAL and Google Scholar were searched for studies reporting on the effect of sarcopenia on postoperative outcomes following oesophageal cancer surgery. Outcomes included surgical complications, anastomotic leakage, respiratory complications, cardiovascular complications, postoperative infections, major complications and overall complications. The random effects model (DerSimonian-Laird) was used to calculate pooled effect estimates when high heterogeneity was encountered, otherwise the fixed-effects (Mantel-Haenszel) model was implemented.
Findings: A total of eight studies involving 1488 patients diagnosed with oesophageal cancer and who underwent oesophagectomy were included in the meta-analysis. The presence of sarcopenia did not significantly increase the rate of surgical complications (odds ratio, OR, 0.86, 95% confidence interval, CI, 0.40-1.85), anastomotic leakage (OR 0.75, 95% CI 0.42-1.35), respiratory complications (OR 0.56, 95% CI 0.21-1.48), cardiovascular complications (OR 0.94, 95% CI 0.31-2.83), postoperative infection (OR 1.14, 95% CI 0.52-2.50), major complications (OR 0.81, 95% CI 0.23-2.82) or overall postoperative complications (OR 0.80, 95% 0.32-1.99).
Conclusion: Sarcopenia does not seem to affect postoperative complication rates of patients undergoing oesophagectomy for oesophageal cancer. Future research should focus on determining whether prognosis differs according to muscle mass in this patient population.
Keywords: Meta-analysis; Oesophageal cancer; Postoperative complications; Sarcopenia.
Figures


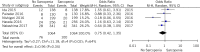

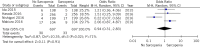


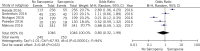
References
-
- McGuckin DG, Mufti S, Turner DJ et al. The association of peri-operative scores, including frailty, with outcomes after unscheduled surgery. Anaesthesia 2018; : 819–824. - PubMed
-
- Copeland GP, Jones D, Walters M. POSSUM: a scoring system for surgical audit. Br J Surg 1991; : 355–360. - PubMed
-
- Fried LP, Tangen CM, Walston J et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 2001; : M146–M156. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

