Physician Perspectives on Deprescribing Cardiovascular Medications for Older Adults
- PMID: 31509233
- PMCID: PMC7061460
- DOI: 10.1111/jgs.16157
Physician Perspectives on Deprescribing Cardiovascular Medications for Older Adults
Abstract
Background/objectives: Guideline-based management of cardiovascular disease often involves prescribing multiple medications, which contributes to polypharmacy and risk for adverse drug events in older adults. Deprescribing is a potential strategy to mitigate these risks. We sought to characterize and compare clinician perspectives regarding deprescribing cardiovascular medications across three specialties.
Design: National cross-sectional survey.
Setting: Ambulatory.
Participants: Random sample of geriatricians, general internists, and cardiologists from the American College of Physicians.
Measurements: Electronic survey assessing clinical practice of deprescribing cardiovascular medications, reasons and barriers to deprescribing, and choice of medications to deprescribe in hypothetical clinical cases.
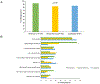
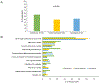
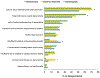
Results: In each specialty, 750 physicians were surveyed, with a response rate of 26% for geriatricians, 26% for general internists, and 12% for cardiologists. Over 80% of respondents within each specialty reported that they had recently considered deprescribing a cardiovascular medication. Adverse drug reactions were the most common reason for deprescribing for all specialties. Geriatricians also commonly reported deprescribing in the setting of limited life expectancy. Barriers to deprescribing were shared across specialties and included concerns about interfering with other physicians' treatment plans and patient reluctance. In hypothetical cases, over 90% of physicians in each specialty chose to deprescribe when patients experienced adverse drug reactions. Geriatricians were most likely and cardiologists were least likely to consider deprescribing cardiovascular medications in cases of limited life expectancy (all P < .001), such as recurrent metastatic cancer (84% of geriatricians, 68% of general internists, and 45% of cardiologists), Alzheimer dementia (92% of geriatricians, 81% of general internists, and 59% of cardiologists), or significant functional impairment (83% of geriatricians, 68% of general internists, and 45% of cardiologists).
Conclusions: While barriers to deprescribing cardiovascular medications are shared across specialties, reasons for deprescribing, especially in the setting of limited life expectancy, varied. Implementing deprescribing will require improved processes for both physician-physician and physician-patient communication. J Am Geriatr Soc 68:78-86, 2019.
Keywords: cardiovascular medications; deprescribing; polypharmacy; variation in care.
© 2019 The American Geriatrics Society.
Figures
Similar articles
-
Deprescribing practices, habits and attitudes of geriatricians and geriatricians-in-training across Europe: a large web-based survey.Eur Geriatr Med. 2022 Dec;13(6):1455-1466. doi: 10.1007/s41999-022-00702-9. Epub 2022 Nov 2. Eur Geriatr Med. 2022. PMID: 36319837 Free PMC article.
-
How general practitioners would deprescribe in frail oldest-old with polypharmacy - the LESS study.BMC Fam Pract. 2018 Oct 12;19(1):169. doi: 10.1186/s12875-018-0856-9. BMC Fam Pract. 2018. PMID: 30314468 Free PMC article.
-
Factors influencing deprescribing habits among geriatricians.Age Ageing. 2015 Jul;44(4):704-8. doi: 10.1093/ageing/afv028. Epub 2015 Mar 10. Age Ageing. 2015. PMID: 25758409
-
Tools for Deprescribing in Frail Older Persons and Those with Limited Life Expectancy: A Systematic Review.J Am Geriatr Soc. 2019 Jan;67(1):172-180. doi: 10.1111/jgs.15616. Epub 2018 Oct 13. J Am Geriatr Soc. 2019. PMID: 30315745
-
Deprescribing in Older Adults With Cardiovascular Disease.J Am Coll Cardiol. 2019 May 28;73(20):2584-2595. doi: 10.1016/j.jacc.2019.03.467. J Am Coll Cardiol. 2019. PMID: 31118153 Free PMC article. Review.
Cited by
-
N-of-1 trials to facilitate evidence-based deprescribing: Rationale and case study.Br J Clin Pharmacol. 2022 Oct;88(10):4460-4473. doi: 10.1111/bcp.15442. Epub 2022 Jul 13. Br J Clin Pharmacol. 2022. PMID: 35705532 Free PMC article. Review.
-
Differences in Factors Influencing Deprescribing between Primary Care Providers: Cross-Sectional Study.Int J Environ Res Public Health. 2023 Mar 11;20(6):4957. doi: 10.3390/ijerph20064957. Int J Environ Res Public Health. 2023. PMID: 36981865 Free PMC article.
-
Deprescribing Cardiovascular Medications in Older Adults Living with Frailty.CJC Open. 2024 Sep 25;6(12):1503-1512. doi: 10.1016/j.cjco.2024.09.008. eCollection 2024 Dec. CJC Open. 2024. PMID: 39735941 Free PMC article. Review.
-
Impact of Supervised Exercise on One-Year Medication Use in Older Veterans with Multiple Morbidities.Gerontol Geriatr Med. 2020 Sep 19;6:2333721420956751. doi: 10.1177/2333721420956751. eCollection 2020 Jan-Dec. Gerontol Geriatr Med. 2020. PMID: 32995368 Free PMC article.
-
Complex and Potentially Harmful Medication Patterns in Heart Failure with Preserved Ejection Fraction.Am J Med. 2021 Mar;134(3):374-382. doi: 10.1016/j.amjmed.2020.07.023. Epub 2020 Aug 18. Am J Med. 2021. PMID: 32822663 Free PMC article.
References
-
- Budnitz DS, Lovegrove MC, Shehab N, et al. Emergency hospitalizations for adverse drug events in older Americans. N Engl J Med. 2011;365(21):2002–2012. - PubMed

