Discovery and Validation of a Biomarker Model (PRESERVE) Predictive of Renal Outcomes After Liver Transplantation
- PMID: 31509263
- PMCID: PMC7883482
- DOI: 10.1002/hep.30939
Discovery and Validation of a Biomarker Model (PRESERVE) Predictive of Renal Outcomes After Liver Transplantation
Abstract
Background and aims: A high proportion of patients develop chronic kidney disease (CKD) after liver transplantation (LT). We aimed to develop clinical/protein models to predict future glomerular filtration rate (GFR) deterioration in this population.
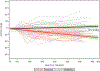
Approach and results: In independent multicenter discovery (CTOT14) and single-center validation (BUMC) cohorts, we analyzed kidney injury proteins in serum/plasma samples at month 3 after LT in recipients with preserved GFR who demonstrated subsequent GFR deterioration versus preservation by year 1 and year 5 in the BUMC cohort. In CTOT14, we also examined correlations between serial protein levels and GFR over the first year. A month 3 predictive model was constructed from clinical and protein level variables using the CTOT14 cohort (n = 60). Levels of β-2 microglobulin and CD40 antigen and presence of hepatitis C virus (HCV) infection predicted early (year 1) GFR deterioration (area under the curve [AUC], 0.814). We observed excellent validation of this model (AUC, 0.801) in the BUMC cohort (n = 50) who had both early and late (year 5) GFR deterioration. At an optimal threshold, the model had the following performance characteristics in CTOT14 and BUMC, respectively: accuracy (0.75, 0.8), sensitivity (0.71, 0.67), specificity (0.78, 0.88), positive predictive value (0.74, 0.75), and negative predictive value (0.76, 0.82). In the serial CTOT14 analysis, several proteins, including β-2 microglobulin and CD40, correlated with GFR changes over the first year.
Conclusions: We have validated a clinical/protein model (PRESERVE) that early after LT can predict future renal deterioration versus preservation with high accuracy. This model may help select recipients at higher risk for subsequent CKD for early, proactive renal sparing strategies.
© 2019 by the American Association for the Study of Liver Diseases.
Figures
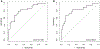

References
-
- Gonwa TA, Mai ML, Melton LB, Hays SR, Goldstein RM, Levy MF, Klintmalm GB. End-stage renal disease (ESRD) after orthotopic liver transplantation (OLTX) using calcineurin-based immunotherapy: risk of development and treatment. Transplantation 2001;72:1934–1939. - PubMed
-
- Velidedeoglu E, Bloom RD, Crawford MD, Desai NM, Campos L, Abt PL, et al. Early kidney dysfunction post liver transplantation predicts late chronic kidney disease. Transplantation 2004;77:553–556. - PubMed
-
- Ojo AO, Held PJ, Port FK, Wolfe RA, Leichtman AB, Young EW, et al. Chronic renal failure after transplantation of a nonrenal organ. N Engl J Med 2003;349:931–940. - PubMed
-
- Schwarz A, Haller H, Schmitt R, Schiffer M, Koenecke C, Strassburg C, et al. Biopsy-diagnosed renal disease in patients after transplantation of other organs and tissues. Am J Transplant 2010;10:2017–2025. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

