Prospective randomized comparison of repairing vesicovaginal fistula with or without the interposition flap: Result from a tertiary care Institute in Northern India
- PMID: 31509511
- PMCID: PMC6739083
- DOI: 10.5152/tud.2019.85233
Prospective randomized comparison of repairing vesicovaginal fistula with or without the interposition flap: Result from a tertiary care Institute in Northern India
Abstract
Objective: Assessment of results of repairing vesicovaginal fistula (VVF) with or without the use of interposition flaps.
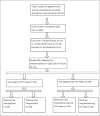
Material and methods: This prospective randomized study was conducted between January 2012 to December 2017 in the Department of Urology, King George's Medical University, Lucknow, India. Obstetric and gynecological simple fistula of ≤4 cm were included for evaluation. Those with complex or complicated fistula or fistula due to malignancy were excluded. Patients were divided into two groups (group 1 and group 2) depending upon route of repair i.e., transvaginal or transabdominal, respectively, as per the characteristics and location of the fistula. These two groups of patients were randomized into two subgroups (1A, 1B and 2A, 2B) based on the inclusion or omission of the interposition flap during fistula repair. Perioperative and postoperative parameters (blood loss, mean operating time, hospital stay, and requirement of analgesics) and success rates of fistula repair were compared. All complications that occurred in the postoperative period till the last follow-up appointment were recorded. The Clavien-Dindo Classification was used to stratify the complications.
Results: Fifty-seven patients underwent transvaginal repair in group 1 (29 with Martius flap: group 1A; 28 without Martius flap: group 1B), while 69 patients underwent transabdominal repair in group 2 (35 with interposition flap: group 2A; 34 without flap: group 2B). Blood loss, mean operating time, hospital stay, and the requirement of analgesics were comparable between each subgroup-1A versus 1B and 2A versus 2B, respectively. The overall success rate of repair across all groups was 96.04% (121/126). The success rate was 93.1% in transvaginal repair with Martius flap versus 96.43% in transvaginal repair with no flap (p=1.0). Success rate was 97.1% in transabdominal repair with an omental flap versus 97.06% in without an omental flap (p=1.0). Mean follow-up period was 39.6 months (range: 6-68 months). Out of 29 patients with Martius flap interposition, 9 (31.03%) of them reported a significantly reduced sensation on the labia majora. Of these 9 patients, 5 reported numbness while the remaining 4 experienced pain as compared to the patients in subgroup IB, who did not report any altered sensation in the labia. (p=0.0019).
Conclusion: The success rates are similar in simple VVF repair (fistula size less than 4 cm) irrespective of the use of interposition flaps. However, overall morbidities following repair with the interposition flap are higher when compared with repair without interposition flap, either by the transvaginal or by the transabdominal route.
Conflict of interest statement
Similar articles
-
Ten-year experience with transvaginal vesicovaginal fistula repair using tissue interposition.J Urol. 2003 Mar;169(3):1033-6. doi: 10.1097/01.ju.0000049723.57485.e7. J Urol. 2003. PMID: 12576839
-
Interposition flaps in vesicovaginal fistula repairs can optimize cure rate.Urol Ann. 2013 Oct;5(4):270-2. doi: 10.4103/0974-7796.120305. Urol Ann. 2013. PMID: 24311909 Free PMC article.
-
Treatment of vesicovaginal fistulas: an experience of 30 cases.Med Arch. 2013;67(4):266-9. doi: 10.5455/medarh.2013.67.266-269. Med Arch. 2013. PMID: 24520750
-
Guidelines of how to manage vesicovaginal fistula.Crit Rev Oncol Hematol. 2003 Dec;48(3):295-304. doi: 10.1016/s1040-8428(03)00123-9. Crit Rev Oncol Hematol. 2003. PMID: 14693342 Review.
-
[Closure of a neobladder-vaginal fistula in a patient with Studer's type neobladder using a transvaginal approach with interposition of a Martius' flap].Arch Esp Urol. 2009 Jan-Feb;62(1):56-9. doi: 10.4321/s0004-06142009000100008. Arch Esp Urol. 2009. PMID: 19400447 Review. Spanish.
Cited by
-
Radiation-Induced Recurrent Vesicovaginal Fistula-Treatment with Adjuvant Platelet-Rich Plasma Injection and Martius Flap Placement-Case Report and Review of Literature.Int J Environ Res Public Health. 2021 May 3;18(9):4867. doi: 10.3390/ijerph18094867. Int J Environ Res Public Health. 2021. PMID: 34063610 Free PMC article. Review.
-
Repair of Vesicovaginal Fistulae: A Systematic Review.Obstet Gynecol. 2024 Feb 1;143(2):229-241. doi: 10.1097/AOG.0000000000005468. Epub 2023 Nov 30. Obstet Gynecol. 2024. PMID: 38033311 Free PMC article.
-
Transvaginal vesicovaginal fistula closure: A retrospective study of 28 cases at a single facility in Japan.Int J Urol. 2023 Jul;30(7):586-591. doi: 10.1111/iju.15181. Epub 2023 Mar 22. Int J Urol. 2023. PMID: 36946367 Free PMC article.
-
Exploring Urinary Tract Injuries in Gynecological Surgery: Current Insights and Future Directions.Healthcare (Basel). 2025 Jul 23;13(15):1780. doi: 10.3390/healthcare13151780. Healthcare (Basel). 2025. PMID: 40805813 Free PMC article. Review.
-
A scoping review of tissue interposition flaps used in vesicovaginal fistulae repair.Ther Adv Urol. 2023 Jun 26;15:17562872231182217. doi: 10.1177/17562872231182217. eCollection 2023 Jan-Dec. Ther Adv Urol. 2023. PMID: 37434758 Free PMC article.
References
-
- Sinha HH, Mishra M. A review of urinary fistulae. J Obstet Gynecol India. 2000;50:79–80.
-
- Leach G, Trockman B. Surgery for vesicovaginal and urethrovaginal fistula and urethral diverticulum. In: Walsh PC, Retik AB, Vaughan ED Jr, et al., editors. Campbell’s Urology. 7th ed. Philadelphia: WB Saunders; 1998. pp. 1135–53.
-
- Kursh E, Morse R, Resnik M, Persky L. Prevention and development of vesicovaginal fistula. Surg Gynecol Obstet. 1988;166:409–12. - PubMed
LinkOut - more resources
Full Text Sources