Heated Humidified High Flow Nasal Cannula (HHHFNC) is not an effective method for initial treatment of Respiratory Distress Syndrome (RDS) versus nasal intermittent mandatory ventilation (NIMV) and nasal continuous positive airway pressure (NCPAP)
- PMID: 31523259
- PMCID: PMC6734667
- DOI: 10.4103/jrms.JRMS_2_19
Heated Humidified High Flow Nasal Cannula (HHHFNC) is not an effective method for initial treatment of Respiratory Distress Syndrome (RDS) versus nasal intermittent mandatory ventilation (NIMV) and nasal continuous positive airway pressure (NCPAP)
Abstract
Background: Noninvasive respiratory support techniques are widely used to treat respiratory distress syndrome (RDS) in preterm infants, and the effectiveness of these methods should be compared. In the current study, nasal continuous positive airway pressure (NCPAP), nasal intermittent mandatory ventilation (NIMV), and heated humidified high-flow nasal cannula (HHHFNC) were compared.
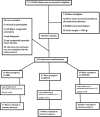
Materials and methods: In the current bicenter clinical trial, 109 preterm infants with RDS not treated with surfactant were randomly assigned to three groups: NCPAP, NIMV, and HHHFNC. The initial outcomes including the failure of treatment within the first initial 72 h, and the duration of RDS treatment, and the secondary outcomes including the need for intubation, the need for surfactants, the duration of oxygen dependency, the incidence of pneumothorax, the patent ductus arteriosus, intraventricular hemorrhage, length of stay, and mortality were compared among the groups.
Results: The frequency of HHHFNC treatment failure (54.3%) was significantly higher compared with those of NIMV (21.6%) (P < 0.001, hazard ratio [HR] = 9.12, 95% confidence interval [CI] = 2.59 - 32.07) and NCPAP (35.1%) (P = 0.004, HR = 21.25, 95% CI = 2.51-180.08). The median duration of RDS treatment was longer (40 h) in the HHHFNC group, although it was not significantly different from those of NIMV (31.16 h) and NCPAP (38.91 h).
Conclusion: Based on the high prevalence of failure of HHHFNC treatment than the other two methods (NCPAP and NIMV), HHHFNC is not recommended as the initial treatment of RDS.
Keywords: Noninvasive ventilation; premature infants; respiratory distress syndrome.
Conflict of interest statement
There are no conflicts of interest.
Figures
References
-
- Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Plavka R, et al. European consensus guidelines on the management of respiratory distress syndrome-2016 update. Neonatology. 2017;111:107–25. - PubMed
-
- Caminita F, van der Merwe M, Hance B, Krishnan R, Miller S, Buddington K, et al. A preterm pig model of lung immaturity and spontaneous infant respiratory distress syndrome. Am J Physiol Lung Cell Mol Physiol. 2015;308:L118–29. - PubMed
-
- Thygesen SK, Olsen M, Pedersen L, Henderson VW, østergaard JR, Sørensen HT. Respiratory distress syndrome in preterm infants and risk of epilepsy in a Danish cohort. Eur J Epidemiol. 2018;33:313–21. - PubMed
-
- Condò V, Cipriani S, Colnaghi M, Bellø R, Zanini R, Bulfoni C, et al. Neonatal respiratory distress syndrome: Are risk factors the same in preterm and term infants? J Matern Fetal Neonatal Med. 2017;30:1267–72. - PubMed