Trends in Survival After Pediatric In-Hospital Cardiac Arrest in the United States
- PMID: 31542952
- PMCID: PMC6803102
- DOI: 10.1161/CIRCULATIONAHA.119.041667
Trends in Survival After Pediatric In-Hospital Cardiac Arrest in the United States
Abstract
Background: Cardiac arrest in hospitalized children is associated with poor outcomes, but no contemporary study has reported whether the trends in survival have changed over time. In this study, we examined temporal trends in survival for pediatric patients with an in-hospital pulseless cardiac arrest and pediatric patients with a nonpulseless cardiopulmonary resuscitation event from 2000 to 2018.
Methods: This was an observational study of hospitalized pediatric patients (≤18 years of age) who received cardiopulmonary resuscitation from January 2000 to December 2018 and were included in the Get With The Guidelines-Resuscitation registry, a United States-based in-hospital cardiac arrest registry. The primary outcome was survival to hospital discharge, and the secondary outcome was return of spontaneous circulation (binary outcomes). Generalized estimation equations were used to obtain unadjusted trends in outcomes over time. Separate analyses were performed for patients with a pulseless cardiac arrest and patients with a nonpulseless event (bradycardia with poor perfusion) requiring cardiopulmonary resuscitation. A subgroup analysis was conducted for shockable versus nonshockable initial rhythms in pulseless events.
Results: A total of 7433 patients with a pulseless cardiac arrest and 5751 patients with a nonpulseless event were included for the analyses. For pulseless cardiac arrests, survival was 19% (95% CI, 11%-29%) in 2000 and 38% (95% CI, 34%-43%) in 2018, with an absolute change of 0.67% (95% CI, 0.40%-0.95%; P<0.001) per year, although the increase in survival appeared to stagnate following 2010. Return of spontaneous circulation also increased over time, with an absolute change of 0.83% (95% CI, 0.53%-1.14%; P<0.001) per year. We found no interaction between survival to hospital discharge and the initial rhythm. For nonpulseless events, survival was 57% (95% CI, 39%-75%) in 2000 and 66% (95% CI, 61%-72%) in 2018, with an absolute change of 0.80% (95% CI, 0.32%-1.27%; P=0.001) per year.
Conclusions: Survival has improved for pediatric events requiring cardiopulmonary resuscitation in the United States, with a 19% absolute increase in survival for in-hospital pulseless cardiac arrests and a 9% absolute increase in survival for nonpulseless events between 2000 and 2018. However, survival from pulseless cardiac arrests appeared to have reached a plateau following 2010.
Keywords: heart arrest; mortality; pediatrics; survival; trends.
Figures


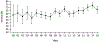
References
-
- Benjamin EJ, Muntner P, Alonso A, Bittencourt MS, Callaway CW, Carson AP, Chamberlain AM, Chang AR, Cheng S, Das SR et al. Heart Disease and Stroke Statistics-2019 Update: A Report From the American Heart Association. Circulation. 2019:CIR0000000000000659. - PubMed
-
- Neumar RW. Doubling Cardiac Arrest Survival by 2020: Achieving the American Heart Association Impact Goal. Circulation. 2016;134:2037–2039. - PubMed
-
- Duff JP, Topjian A, Berg MD, Chan M, Haskell SE, Joyner BL, Lasa JJ, Ley SJ, Raymond TT, Sutton RM et al. 2018 American Heart Association Focused Update on Pediatric Advanced Life Support: An Update to the American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2018;138:e731–e739. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

