Renal and pulmonary thrombotic microangiopathy triggered by proteasome-inhibitor therapy in patient with smoldering myeloma: A renal biopsy and autopsy case report
- PMID: 31574818
- PMCID: PMC6775360
- DOI: 10.1097/MD.0000000000017148
Renal and pulmonary thrombotic microangiopathy triggered by proteasome-inhibitor therapy in patient with smoldering myeloma: A renal biopsy and autopsy case report
Abstract
Rationale: Thrombotic microangiopathy (TMA) is a group of clinical syndromes characterized by excessive platelet activation and endothelial injury that leads to acute or chronic microvascular obliteration by intimal mucoid and fibrous thickening, with or without associated thrombi. It frequently involves the kidney but may involve any organ or system at variable frequencies depending on the underlying etiology. Among its numerous causes, drug toxicities and complement regulation abnormalities stand out as some of the most common. A more recently described association is with monoclonal gammopathy. Lung involvement by TMA is infrequent, but has been described in Cobalamin C deficiency and post stem-cell transplantation TMA.
Patient concerns: This is the case of a patient with smoldering myeloma who received proteasome-inhibitor therapy due to retinopathy and developed acute renal failure within one week of therapy initiation.
Diagnoses: A renal biopsy showed thrombotic microangiopathy. At the time, mild pulmonary hypertension was also noted and presumed to be idiopathic.
Interventions: Given the known association of proteasome-inhibitor therapy with thrombotic microangiopathy, Bortezomib was discontinued and dialysis was initiated.
Outcomes: Drug withdrawal failed to prevent disease progression and development of end-stage renal disease, as well as severe pulmonary hypertension that eventually lead to the patient's death.
Lessons: To our knowledge, this is the first reported case of pulmonary involvement by TMA associated with monoclonal gammopathy which appears to have been triggered by proteasome-inhibitor therapy. Clinicians should be aware of this possibility to allow for more prompt recognition of pulmonary hypertension as a potential manifestation of monoclonal gammopathy-associated TMA, especially in patients also receiving proteasome-inhibitors, so that treatment aiming to slow disease progression can be instituted.
Conflict of interest statement
The authors of this case report have no conflicts of interest to disclose.
Figures
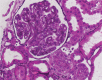
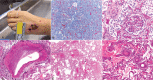
Similar articles
-
Renal thrombotic microangiopathy and podocytopathy associated with the use of carfilzomib in a patient with multiple myeloma.BMC Nephrol. 2014 Sep 30;15:156. doi: 10.1186/1471-2369-15-156. BMC Nephrol. 2014. PMID: 25267524 Free PMC article.
-
Thrombotic microangiopathy associated with monoclonal gammopathy.Kidney Int. 2017 Mar;91(3):691-698. doi: 10.1016/j.kint.2016.09.045. Epub 2016 Dec 18. Kidney Int. 2017. PMID: 27998645
-
Microangiopathy in multiple myeloma: a case of carfilzomib-induced secondary thrombotic microangiopathy successfully treated with plasma exchange and complement inhibition.BMC Nephrol. 2023 Jun 19;24(1):179. doi: 10.1186/s12882-023-03228-9. BMC Nephrol. 2023. PMID: 37337151 Free PMC article.
-
Drug-induced Thrombotic Microangiopathy with Concurrent Proteasome Inhibitor Use in the Treatment of Multiple Myeloma: A Case Series and Review of the Literature.Clin Lymphoma Myeloma Leuk. 2020 Nov;20(11):e791-e800. doi: 10.1016/j.clml.2020.04.014. Epub 2020 Apr 30. Clin Lymphoma Myeloma Leuk. 2020. PMID: 32807717 Review.
-
Clinicopathological spectrum of kidney diseases in cancer patients treated with vascular endothelial growth factor inhibitors: a report of 5 cases and review of literature.Hum Pathol. 2014 Sep;45(9):1918-27. doi: 10.1016/j.humpath.2014.05.015. Epub 2014 Jun 12. Hum Pathol. 2014. PMID: 25087655 Review.
Cited by
-
Carfilzomib-induced atypical haemolytic uraemic syndrome: a diagnostic challenge and therapeutic success.BMJ Case Rep. 2021 Feb 26;14(2):e239091. doi: 10.1136/bcr-2020-239091. BMJ Case Rep. 2021. PMID: 33637496 Free PMC article.
-
An Update in Drug-Induced Thrombotic Microangiopathy.Front Med (Lausanne). 2020 May 22;7:212. doi: 10.3389/fmed.2020.00212. eCollection 2020. Front Med (Lausanne). 2020. PMID: 32528969 Free PMC article. No abstract available.
-
Cancer Therapy-Associated Pulmonary Hypertension and Right Ventricular Dysfunction: Etiologies and Prognostic Implications.Rev Cardiovasc Med. 2024 Mar 5;25(3):87. doi: 10.31083/j.rcm2503087. eCollection 2024 Mar. Rev Cardiovasc Med. 2024. PMID: 39076943 Free PMC article. Review.
-
Pulmonary hypertension in patients with multiple myeloma: A comprehensive review.Pulm Circ. 2023 Apr 1;13(2):e12210. doi: 10.1002/pul2.12210. eCollection 2023 Apr. Pulm Circ. 2023. PMID: 37063748 Free PMC article. Review.
-
Proteasome inhibitor-associated thrombotic microangiopathy: a real-world retrospective and pharmacovigilance database analysis.Support Care Cancer. 2025 Feb 13;33(3):184. doi: 10.1007/s00520-025-09219-w. Support Care Cancer. 2025. PMID: 39939437
References
-
- Goodship TH, Cook HT, Fakhouri F, et al. Atypical hemolytic uremic syndrome and C3 glomerulopathy: conclusions from a “Kidney Disease: Improving Global Outcomes” (KDIGO) Controversies Conference. Kidney Int 2017;91:539–51. - PubMed
-
- Grangé S, Bekri S, Artaud-Macari E, et al. Adult-onset renal thrombotic microangiopathy and pulmonary arterial hypertension in cobalamin C deficiency. Lancet 2015;386:1011–2. - PubMed
-
- Komhoff M, Roofthooft MT, Westra D, et al. Combined pulmonary hypertension and renal thrombotic microangiopathy in cobalamin C deficiency. Pediatrics 2013;132:e540–4. - PubMed
-
- Jodele S, Hirsch R, Laskin B, et al. Pulmonary arterial hypertension in pediatric patients with hematopoietic stem cell transplant-associated thrombotic microangiopathy. Biol Blood Marrow Transplant 2013;19:202–7. - PubMed
-
- Yui JC, Van Keer J, Weiss BM, et al. Proteasome inhibitor associated thrombotic microangiopathy. Am J Hematol 2016;91:E348–52. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

