Impact of Body Composition on the Risk of Hepatocellular Carcinoma Recurrence After Liver Transplantation
- PMID: 31614892
- PMCID: PMC6832484
- DOI: 10.3390/jcm8101672
Impact of Body Composition on the Risk of Hepatocellular Carcinoma Recurrence After Liver Transplantation
Abstract
Background: Body composition parameters are reported to influence the risk of hepatocellular carcinoma (HCC) recurrence after liver resection, yet data on patients undergoing liver transplantation are scarce. The aim of this study was to evaluate the impact of the amount of abdominal adipose tissue and skeletal muscles on the risk of HCC recurrence after liver transplantation.
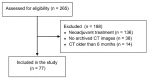
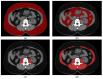
Methods: This was a retrospective observational study performed on 77 HCC patients after liver transplantation. Subcutaneous fat area (SFA), visceral fat area, psoas muscle area and total skeletal muscle area were assessed on computed tomography on the level of L3 vertebra and divided by square meters of patient height. The primary outcome measure was five-year recurrence-free survival.
Results: Recurrence-free survival in the entire cohort was 95.7%, 90.8%, and 86.5% after one, three, and five years post-transplantation, respectively. SFA was significantly associated with the risk of HCC recurrence (p = 0.013), whereas no significant effects were found for visceral fat and skeletal muscle indices. The optimal cut-off for SFA for prediction of recurrence was 71.5 cm2/m2. Patients with SFA < 71.5 cm2/m2 and ≥71.5 cm2/m2 exhibited five-year recurrence-free survival of 96.0% and 55.4%, respectively (p = 0.001).
Conclusions: Excessive amount of subcutaneous adipose tissue is a risk factor for HCC recurrence after liver transplantation and may be considered in patient selection process.
Keywords: adipose tissue; computed tomography; hepatocellular carcinoma; liver transplantation; obesity; sarcopenia; subcutaneous fat; visceral fat.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

Similar articles
-
Visceral adiposity increases risk for hepatocellular carcinoma in male patients with cirrhosis and recurrence after liver transplant.Hepatology. 2018 Mar;67(3):914-923. doi: 10.1002/hep.29578. Epub 2018 Jan 26. Hepatology. 2018. PMID: 29023899
-
Increased visceral fat volume raises the risk for recurrence of hepatocellular carcinoma after curative treatment.Oncotarget. 2018 Feb 16;9(18):14058-14067. doi: 10.18632/oncotarget.24500. eCollection 2018 Mar 6. Oncotarget. 2018. PMID: 29581826 Free PMC article.
-
Impact of Sarcopenic Obesity on Outcomes in Patients Undergoing Hepatectomy for Hepatocellular Carcinoma.Ann Surg. 2019 May;269(5):924-931. doi: 10.1097/SLA.0000000000002555. Ann Surg. 2019. PMID: 29064889
-
Sarcopenia and chronic liver diseases.Expert Rev Gastroenterol Hepatol. 2018 Dec;12(12):1229-1244. doi: 10.1080/17474124.2018.1534586. Epub 2018 Oct 16. Expert Rev Gastroenterol Hepatol. 2018. PMID: 30791794 Review.
-
Imaging based body composition profiling and outcomes after oncologic liver surgery.Front Oncol. 2022 Dec 8;12:1007771. doi: 10.3389/fonc.2022.1007771. eCollection 2022. Front Oncol. 2022. PMID: 36568174 Free PMC article. Review.
Cited by
-
Impact of CT-relevant skeletal muscle parameters on post-liver transplantation survival in patients with hepatocellular carcinoma.Hepatol Int. 2024 Oct;18(5):1516-1527. doi: 10.1007/s12072-024-10708-z. Epub 2024 Jul 14. Hepatol Int. 2024. PMID: 39003652
-
Development and validation of a clinical factors and body fat distribution-based nomogram to predict refractoriness of transarterial chemoembolization in hepatocellular carcinoma.Quant Imaging Med Surg. 2024 Jan 3;14(1):447-461. doi: 10.21037/qims-23-963. Epub 2023 Nov 13. Quant Imaging Med Surg. 2024. PMID: 38223027 Free PMC article.
-
Clinically Evident Portal Hypertension Is an Independent Risk Factor of Hepatocellular Carcinoma Recurrence Following Liver Transplantation.J Clin Med. 2025 Mar 17;14(6):2032. doi: 10.3390/jcm14062032. J Clin Med. 2025. PMID: 40142840 Free PMC article.
-
Usefulness of Different Imaging Modalities in Evaluation of Patients with Non-Alcoholic Fatty Liver Disease.Biomedicines. 2020 Aug 21;8(9):298. doi: 10.3390/biomedicines8090298. Biomedicines. 2020. PMID: 32839409 Free PMC article. Review.
-
Sarcopenia defined by psoas muscle index independently predicts long-term survival after living donor liver transplantation in male recipients.Quant Imaging Med Surg. 2022 Jan;12(1):215-228. doi: 10.21037/qims-21-314. Quant Imaging Med Surg. 2022. PMID: 34993073 Free PMC article.
References
-
- Puigvehí M., Hashim D., Haber P.K., Dinani A., Schiano T.D., Asgharpour A., Kushner T., Kakked G., Tabrizian P., Schwartz M., et al. Liver Transplant for Hepatocellular Carcinoma in the United States: Evolving Trends over the Last Three Decades. Am. J. Transplant. 2019 doi: 10.1111/ajt.15576. - DOI - PMC - PubMed
-
- Mazzaferro V., Regalia E., Doci R., Andreola S., Pulvirenti A., Bozzetti F., Montalto F., Ammatuna M., Morabito A., Gennari L. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N. Engl. J. Med. 1996;334:693–699. doi: 10.1056/NEJM199603143341104. - DOI - PubMed
-
- Grąt M., Wronka K.M., Stypułkowski J., Bik E., Krasnodębski M., Masior Ł., Lewandowski Z., Grąt K., Patkowski W., Krawczyk M. The Warsaw Proposal for the Use of Extended Selection Criteria in Liver Transplantation for Hepatocellular Cancer. Ann. Surg. Oncol. 2017;24:526–534. doi: 10.1245/s10434-016-5500-0. - DOI - PMC - PubMed
-
- Mazzaferro V., Sposito C., Zhou J., Pinna A.D., De Carlis L., Fan J., Cescon M., Di Sandro S., Yi-Feng H., Lauterio A., et al. Metroticket 2.0 Model for Analysis of Competing Risks of Death After Liver Transplantation for Hepatocellular Carcinoma. Gastroenterology. 2018;154:128–139. doi: 10.1053/j.gastro.2017.09.025. - DOI - PubMed
-
- Duvoux C., Roudot-Thoraval F., Decaens T., Pessione F., Badran H., Piardi T., Francoz C., Compagnon P., Vanlemmens C., Dumortier J., et al. Liver transplantation for hepatocellular carcinoma: A model including α-Fetoprotein improves the performance of Milan criteria. Gastroenterology. 2012;143:986–994. doi: 10.1053/j.gastro.2012.05.052. - DOI - PubMed
LinkOut - more resources
Full Text Sources

