Evolving concepts in bone infection: redefining "biofilm", "acute vs. chronic osteomyelitis", "the immune proteome" and "local antibiotic therapy"
- PMID: 31646012
- PMCID: PMC6804538
- DOI: 10.1038/s41413-019-0061-z
Evolving concepts in bone infection: redefining "biofilm", "acute vs. chronic osteomyelitis", "the immune proteome" and "local antibiotic therapy"
Abstract
Osteomyelitis is a devastating disease caused by microbial infection of bone. While the frequency of infection following elective orthopedic surgery is low, rates of reinfection are disturbingly high. Staphylococcus aureus is responsible for the majority of chronic osteomyelitis cases and is often considered to be incurable due to bacterial persistence deep within bone. Unfortunately, there is no consensus on clinical classifications of osteomyelitis and the ensuing treatment algorithm. Given the high patient morbidity, mortality, and economic burden caused by osteomyelitis, it is important to elucidate mechanisms of bone infection to inform novel strategies for prevention and curative treatment. Recent discoveries in this field have identified three distinct reservoirs of bacterial biofilm including: Staphylococcal abscess communities in the local soft tissue and bone marrow, glycocalyx formation on implant hardware and necrotic tissue, and colonization of the osteocyte-lacuno canalicular network (OLCN) of cortical bone. In contrast, S. aureus intracellular persistence in bone cells has not been substantiated in vivo, which challenges this mode of chronic osteomyelitis. There have also been major advances in our understanding of the immune proteome against S. aureus, from clinical studies of serum antibodies and media enriched for newly synthesized antibodies (MENSA), which may provide new opportunities for osteomyelitis diagnosis, prognosis, and vaccine development. Finally, novel therapies such as antimicrobial implant coatings and antibiotic impregnated 3D-printed scaffolds represent promising strategies for preventing and managing this devastating disease. Here, we review these recent advances and highlight translational opportunities towards a cure.
Keywords: Bone; Diseases.
© The Author(s) 2019.
Conflict of interest statement
Competing interestsThe authors declare no competing interests.
Figures




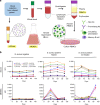
References
-
- Peltola H, Pääkkönen M, Kallio P, Kallio MJ, Group O-SAS. Short-versus long-term antimicrobial treatment for acute hematogenous osteomyelitis of childhood: prospective, randomized trial on 131 culture-positive cases. Pediatr. Infect. Dis. J. 2010;29:1123–1128. doi: 10.1097/INF.0b013e3181f55a89. - DOI - PubMed
-
- Steiner, C., Andrews, R., Barrett, M., Weiss, A. US Agency for Healthcare Research and Quality; 2012. HCUP projections: mobility/orthopedic procedures 2003 to 2012. Report# 2012-03 (2014).
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

