Coronal magnetic resonance imaging of three-dimensional fast-field echo with water-selective excitation improves the sensitivity and reliability of identification of extraforaminal lumbar disc herniation
- PMID: 31662019
- PMCID: PMC7045647
- DOI: 10.1177/0300060519882546
Coronal magnetic resonance imaging of three-dimensional fast-field echo with water-selective excitation improves the sensitivity and reliability of identification of extraforaminal lumbar disc herniation
Abstract
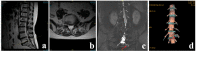
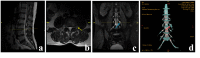
Objective: The complete view of the nerve root, including the extraforaminal zone, can be displayed by coronal magnetic resonance imaging (MRI) of three-dimensional (3D) fast-field echo with water-selective excitation (CMRI). However, its sensitivity, specificity, and reliability for the diagnosis of extraforaminal lumbar disc herniation are unclear. We compared the sensitivity, specificity, and reliability of conventional MRI, CMRI, and 3D MRI for the identification of extraforaminal lumbar disc herniation.
Methods: This study involved 140 patients (68 with extraforaminal lumbar disc herniation and 72 with paramedian disc herniation). Their mean age was 44.57 ± 14.59 years. Conventional MRI, CMRI, and 3D MRI of all patients were evaluated by five experts. The reliability, sensitivity, and specificity of the three imaging techniques for identification of extraforaminal lumbar disc herniation were compared using kappa statistics and the chi-squared test.
Results: CMRI showed higher agreement (0.843) than conventional MRI (0.671) and 3D MRI (0.771) for the identification of extraforaminal lumbar disc herniation. CMRI demonstrated higher sensitivity (95.6% vs. 91.2%) than conventional MRI (85.3% vs. 70.6%) and 3D MRI (92.6% vs. 86.7%) regardless of whether performed by junior or senior surgeons.
Conclusions: CMRI is helpful for identification of extraforaminal disc herniation by junior and senior orthopedic surgeons.
Keywords: Extraforaminal herniation; magnetic resonance imaging; reliability; sciatica; sensitivity; specificity.
Figures

References
-
- Baek J, Yang SH, Kim CH, et al. Postoperative longitudinal outcomes in patients with residual disc fragments after percutaneous endoscopic lumbar discectomy. Pain Physician 2018; 21: E457–E466. - PubMed
-
- Wang Y, Zhang W, Lian L, et al. Transforaminal endoscopic discectomy for treatment of central disc herniation: surgical techniques and clinical outcome. Pain Physician 2018; 21: E113–E123. - PubMed
-
- Akinduro OO, Kerezoudis P, Alvi MA, et al. Open versus minimally invasive surgery for extraforaminal lumbar disk herniation: a systematic review and meta-analysis. World Neurosurg 2017; 108: 924–938.e3. - PubMed
MeSH terms
Supplementary concepts
LinkOut - more resources
Full Text Sources
Medical

