Healthcare Policy Changes in Osteoporosis Can Improve Outcomes and Reduce Costs in the United States
- PMID: 31667450
- PMCID: PMC6808223
- DOI: 10.1002/jbm4.10192
Healthcare Policy Changes in Osteoporosis Can Improve Outcomes and Reduce Costs in the United States
Abstract
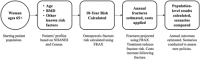
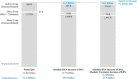
In the United States, osteoporosis affects over 10 million adults, has high societal costs ($22 billion in 2008), and is currently being underdiagnosed and undertreated. Given an aging population, this burden is expected to rise. We projected the fracture burden in US women by modeling the expected demographic shift as well as potential policy changes. With the anticipated population aging and growth, annual fractures are projected to increase from 1.9 million to 3.2 million (68%), from 2018 to 2040, with related costs rising from $57 billion to over $95 billion. Policy-driven expansion of case finding and treatment of at-risk women could lower this burden, preventing 6.1 million fractures over the next 22 years while reducing payer costs by $29 billion and societal costs by $55 billion. Increasing use of osteoporosis-related interventions can reduce fractures and result in substantial cost-savings, a rare and fortunate combination given the current landscape in healthcare policy. © 2019 The Authors. JBMR Plus published by Wiley Periodicals, Inc. on behalf of American Society for Bone and Mineral Research.
Keywords: FRACTURE PREVENTION; FRACTURE RISK ASSESSMENT; GENERAL POPULATION STUDIES; HEALTH ECONOMICS; OSTEOPOROSIS.
© 2019 The Authors. JBMR Plus published by Wiley Periodicals, Inc. on behalf of American Society for Bone and Mineral Research.
Figures

References
-
- King AB, Fiorentino DM. Medicare payment cuts for osteoporosis testing reduced use despite tests’ benefit in reducing fractures. Health Aff (Millwood) 2011;30(12):2362–70. - PubMed
-
- Lewiecki EM, Adler R, Curtis Jet al. Hip fractures and declining DXA testing: at a breaking point? J Bone Miner Res 2016;31(S1):S1–411.
LinkOut - more resources
Full Text Sources
