How much do hospitalized adults move? A systematic review and meta-analysis
- PMID: 31672262
- PMCID: PMC7051878
- DOI: 10.1016/j.apnr.2019.151189
How much do hospitalized adults move? A systematic review and meta-analysis
Abstract
Aim: To quantify the type and duration of physical activity performed by hospitalized adults.
Background: Inactivity is pervasive among hospitalized patients and is associated with increased mortality, functional decline, and cognitive impairment. Objective measurement of activity is necessary to examine associations with clinical outcomes and quantify optimal inpatient mobility interventions.
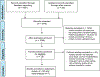
Methods: We used PRISMA guidelines to search three databases in December 2017 to retrieve original research evaluating activity type and duration among adult acute-care inpatients. We abstracted data on inpatient population, measurement method, monitoring time, activity duration, and study quality.
Results: Thirty-eight articles were included in the review and 7 articles were included in the meta-analysis. Study populations included geriatric (n = 5), surgical (n = 5), medical (n = 12), post-stroke (n = 10), psychiatric (n = 2), and critical care inpatients (n = 4). To measure activity, 29% of studies used human observation and 71% used activity monitors. Among inpatient populations, 87-100% of time was spent sitting or lying in-bed. Among medical inpatients monitored over a continuous 24-hour period (n = 7), 70 min per day was spent standing/walking (95% CI 57-83 min).
Conclusions: This review provides a baseline assessment and benchmark of inpatient activity, which can be used to compare inpatient mobility practices. While there is substantial heterogeneity in how researchers measure and define how much inpatients move, there is consistent evidence that patients are mostly inactive and in-bed during hospitalization. Future research is needed to establish standardized methods to accurately and consistently measure inpatient mobility over time.
Keywords: Early mobility; Fitness tracker; Hospitalization; Physical activity; Systematic review.
Copyright © 2019 Elsevier Inc. All rights reserved.
Conflict of interest statement
Declaration of Conflicting Interests
Dr. Fazio reports receipt of research equipment donated by Leaf Healthcare Inc. outside of the submitted work. This review was conceived and designed independently of funders who had no role in data collection, analysis or writing of manuscripts.
Figures


References
-
- Creditor MC. Hazards of hospitalization of the elderly. Annals of internal medicine 1993;118(3):219–23. - PubMed
-
- Brown CJ, Friedkin RJ, Inouye SK. Prevalence and outcomes of low mobility in hospitalized older patients. Journal of the American Geriatrics Society 2004;52(8):1263–70. - PubMed
-
- Zisberg A, Shadmi E, Sinoff G, Gur-Yaish N, Srulovici E, Admi H. Low mobility during hospitalization and functional decline in older adults. Journal of the American Geriatrics Society 2011;59(2):266–73. - PubMed
-
- Griffiths RD, Hall JB. Intensive care unit-acquired weakness. Critical care medicine 2010;38(3):779–87. - PubMed
-
- Winkelman C Bed rest in health and critical illness: a body systems approach. AACN advanced critical care 2009;20(3):254–66. - PubMed

