Treatment Outcome of 227 Patients with Sinonasal Adenoid Cystic Carcinoma (ACC) after Intensity Modulated Radiotherapy and Active Raster-Scanning Carbon Ion Boost: A 10-Year Single-Center Experience
- PMID: 31683896
- PMCID: PMC6895865
- DOI: 10.3390/cancers11111705
Treatment Outcome of 227 Patients with Sinonasal Adenoid Cystic Carcinoma (ACC) after Intensity Modulated Radiotherapy and Active Raster-Scanning Carbon Ion Boost: A 10-Year Single-Center Experience
Abstract
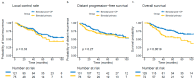
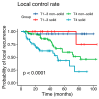
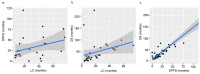
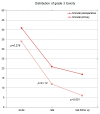
We aimed to evaluate the treatment outcome of primary and postoperative bimodal radiotherapy (RT) including intensity modulated photon radiotherapy (IMRT) and carbon ion radiotherapy (CIRT) for sinonasal adenoid cystic carcinoma (ACC) patients. Medical records of 227 consecutive patients who received either a primary (n = 90, 40%) or postoperative (n = 137, 60%; R2, n = 86, 63%) IMRT with doses between 48 and 56 Gy in 1.8 or 2 Gy fractions and active raster-scanning carbon ion boost with 18 to 24 Gy (RBE, relative biological effectiveness) in 3 Gy (RBE) fractions between 2009 and 2019 up to a median total dose of 80 Gy (EQD2, equivalent dose in 2 Gy single dose fractions, range 71-80 Gy) were reviewed. Results: Median follow-up was 50 months. In univariate and multivariate analysis, no significant difference in local control (LC) could be shown between the two treatment groups (p = 0.33). Corresponding 3-year LC rates were 79% for primary bimodal RT and 82% for postoperative bimodal RT, respectively. T4 stage (p = 0.002) and solid histology (p = 0.005) were identified as independent prognostic factors for decreased LC. Significant worse long-term treatment tolerance was observed for postoperatively irradiated patients with 17% vs. 6% late grade 3 toxicity (p < 0.001). Primary radiotherapy including IMRT and carbon ion boost for dose-escalation results in adequate LC with less long-term grade 3 toxicity compared to postoperative bimodal radiotherapy in sinonasal ACC patients. The high rate of macroscopic tumor disease in the postoperative group makes the interpretation of the beneficial results in LC for primary RT difficult.
Keywords: adenoid cystic carcinoma; carbon ion radiotherapy; local control; recurrence patterns; sinonasal carcinoma; toxicity.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Comment in
-
Managing locally advanced adenoid cystic carcinoma of the head and neck during the COVID-19 pandemic crisis: Is this the right time for particle therapy?Oral Oncol. 2020 Jul;106:104803. doi: 10.1016/j.oraloncology.2020.104803. Epub 2020 May 14. Oral Oncol. 2020. PMID: 32410826 Free PMC article. No abstract available.
References
-
- Chen A.M., Bucci M.K., Weinberg V., Garcia J., Quivey J.M., Schechter N.R., Phillips T.L., Fu K.K., Eisele D.W. Adenoid cystic carcinoma of the head and neck treated by surgery with or without postoperative radiation therapy: Prognostic features of recurrence. Int. J. Radiat. Oncol. Biol. Phys. 2006;66:152–159. doi: 10.1016/j.ijrobp.2006.04.014. - DOI - PubMed
LinkOut - more resources
Full Text Sources

