Disentangling the Gordian knot of local metabolic control of coronary blood flow
- PMID: 31702972
- PMCID: PMC7199237
- DOI: 10.1152/ajpheart.00325.2019
Disentangling the Gordian knot of local metabolic control of coronary blood flow
Abstract
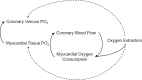
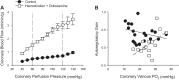
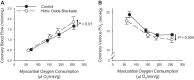
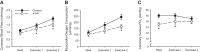
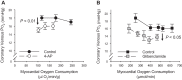
Recognition that coronary blood flow is tightly coupled with myocardial metabolism has been appreciated for well over half a century. However, exactly how coronary microvascular resistance is tightly coupled with myocardial oxygen consumption (MV̇o2) remains one of the most highly contested mysteries of the coronary circulation to this day. Understanding the mechanisms responsible for local metabolic control of coronary blood flow has been confounded by continued debate regarding both anticipated experimental outcomes and data interpretation. For a number of years, coronary venous Po2 has been generally accepted as a measure of myocardial tissue oxygenation and thus the classically proposed error signal for the generation of vasodilator metabolites in the heart. However, interpretation of changes in coronary venous Po2 relative to MV̇o2 are quite nuanced, inherently circular in nature, and subject to confounding influences that remain largely unaccounted for. The purpose of this review is to highlight difficulties in interpreting the complex interrelationship between key coronary outcome variables and the arguments that emerge from prior studies performed during exercise, hemodilution, hypoxemia, and alterations in perfusion pressure. Furthermore, potential paths forward are proposed to help to facilitate further dialogue and study to ultimately unravel what has become the Gordian knot of the coronary circulation.
Keywords: coronary circulation; coronary venous Po2; local metabolic control; myocardial oxygen consumption.
Conflict of interest statement
No conflicts of interest, financial or otherwise, are declared by the authors.
Figures



References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

