Return to work after critical illness: a systematic review and meta-analysis
- PMID: 31704795
- PMCID: PMC7418481
- DOI: 10.1136/thoraxjnl-2019-213803
Return to work after critical illness: a systematic review and meta-analysis
Abstract
Background: Survivors of critical illness often experience poor outcomes after hospitalisation, including delayed return to work, which carries substantial economic consequences.
Objective: To conduct a systematic review and meta-analysis of return to work after critical illness.
Methods: We searched PubMed, Embase, PsycINFO, CINAHL and Cochrane Library from 1970 to February 2018. Data were extracted, in duplicate, and random-effects meta-regression used to obtain pooled estimates.
Results: Fifty-two studies evaluated return to work in 10 015 previously employed survivors of critical illness, over a median (IQR) follow-up of 12 (6.25-38.5) months. By 1-3, 12 and 42-60 months' follow-up, pooled return to work prevalence (95% CI) was 36% (23% to 49%), 60% (50% to 69%) and 68% (51% to 85%), respectively (τ2=0.55, I2=87%, p=0.03). No significant difference was observed based on diagnosis (acute respiratory distress syndrome (ARDS) vs non-ARDS) or region (Europe vs North America vs Australia/New Zealand), but was observed when comparing mode of employment evaluation (in-person vs telephone vs mail). Following return to work, 20%-36% of survivors experienced job loss, 17%-66% occupation change and 5%-84% worsening employment status (eg, fewer work hours). Potential risk factors for delayed return to work include pre-existing comorbidities and post-hospital impairments (eg, mental health).
Conclusion: Approximately two-thirds, two-fifths and one-third of previously employed intensive care unit survivors are jobless up to 3, 12 and 60 months following hospital discharge. Survivors returning to work often experience job loss, occupation change or worse employment status. Interventions should be designed and evaluated to reduce the burden of this common and important problem for survivors of critical illness.
Trial registration number: PROSPERO CRD42018093135.
Keywords: ARDS; clinical epidemiology; critical care.
© Author(s) (or their employer(s)) 2020. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures
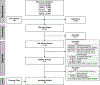

References
-
- Elliott D, Davidson JE, Harvey MA, Bemis-Dougherty A, Hopkins RO, Iwashyna TJ, et al. Exploring the scope of post-intensive care syndrome therapy and care: engagement of non-critical care providers and survivors in a second stakeholders meeting. CritCare Med 2014;42:2518–26. - PubMed
-
- Needham DM, Davidson J, Cohen H, Hopkins RO, Weinert C, Wunsch H, et al. Improving long-term outcomes after discharge from intensive care unit: report from a stakeholders’ conference. CritCare Med 2012;40:502–9. - PubMed
-
- Coopersmith CM, Wunsch H, Fink MP, Linde-Zwirble WT, Olsen KM, Sommers MS, et al. A comparison of critical care research funding and the financial burden of critical illness in the United States. CritCare Med 2012;40:1072–9. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
