Colorectal cancer screening for patients with a family history of colorectal cancer or adenomas
- PMID: 31722908
- PMCID: PMC6853346
Colorectal cancer screening for patients with a family history of colorectal cancer or adenomas
Abstract
Objective: To review and summarize the recently developed Canadian Association of Gastroenterology screening recommendations for patients with a family history of colorectal cancer (CRC) or adenoma from a family medicine perspective.
Quality of evidence: A systematic review and meta-analysis was performed to synthesize knowledge regarding family history and CRC. The Cochrane Central Register of Controlled Trials, MEDLINE, and EMBASE were searched with the following MeSH terms: colorectal cancers or neoplasms, screen or screening or surveillance, and family or family history. Known hereditary syndromes were excluded. The Grading of Recommendations Assessment, Development and Evaluation methodology was used to establish certainty in reviewed evidence. Most recommendations are conditional recommendations with very low-quality evidence.
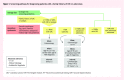
Main message: Individuals who have 1 first-degree relative (FDR) with CRC or an advanced adenoma diagnosed at any age are recommended to undergo colonoscopy every 5 to 10 years starting at age 40 to 50 years or 10 years younger than the age at diagnosis of the FDR, although fecal immunochemical testing at an interval of every 1 to 2 years can be used. Individuals with FDRs with non-advanced adenomas or a history of CRC in second-degree relatives should be screened according to average-risk guidelines. Lifestyle modification can statistically significantly decrease risk of CRC and should be considered in all patients.
Conclusion: These guidelines acknowledge the many factors that can increase an individual's risk of developing CRC and allow for judgment to be employed depending on the clinical scenario. Lifestyle advice already given to patients for weight, blood pressure, and heart disease management will reduce the risk of CRC if implemented, and this combined with more targeted screening for higher-risk individuals will hopefully be successful in decreasing CRC mortality in Canada.
Objectif: Passer en revue et résumer les recommandations récemment élaborées par l’Association canadienne de gastroentérologie pour les patients qui ont des antécédents familiaux de cancer colorectal (CCR) ou d’adénomes, et ce, sous l’angle de la médecine familiale.
Qualité des données: Nous avons procédé à une revue systématique et à une méta-analyse pour faire la synthèse des connaissances concernant les antécédents familiaux et le CCR. Une recension a été effectuée dans le registre central des études contrôlées de Cochrane, MEDLINE et EMBASE, à l’aide des expressions MeSH suivantes : colorectal cancers or neoplasms, screen or screening or surveillance et family or family history. Les syndromes héréditaires connus ont été exclus. La méthodologie GRADE (Grading of Recommendations Assessment, Development and Evaluation) a servi à établir la certitude dans l’examen des données probantes. La majorité des recommandations étaient conditionnelles, s’appuyant sur des données de très faible qualité.
Message principal: Il est recommandé que les personnes dont 1 parent du premier degré (PPD) a ou a eu un CCR ou un adénome avancé diagnostiqué à n’importe quel âge subissent une colonoscopie tous les 5 à 10 ans à partir de 40 à 50 ans, ou 10 ans plus tôt que l’âge au moment du diagnostic du PPD, quoiqu’un test immunochimique fécal puisse être utilisé chaque année ou 2. Les personnes qui ont un PPD sans adénome au stade avancé ou celles qui ont des antécédents familiaux de CCR venant de parents du deuxième degré devraient subir un dépistage selon les lignes directrices s’appliquant à un risque moyen. Les modifications au mode de vie peuvent diminuer le risque de CCR de manière statistiquement significative et devraient être envisagées pour tous les patients.
Conclusion: Ces lignes directrices reconnaissent que de nombreux facteurs peuvent augmenter les risques d’une personne de contracter un CCR et laissent place à l’exercice du jugement en fonction du scénario clinique. Les conseils sur le mode de vie déjà donnés aux patients en matière de poids, de pression artérielle et de prise en charge des cardiopathies réduiront le risque de CCR s’ils sont suivis. La mise en pratique de ces conseils, de même qu’un dépistage plus ciblé pour les personnes à risque plus élevé, devraient réussir à réduire la mortalité due au CCR au Canada.
Copyright© the College of Family Physicians of Canada.
Figures
References
-
- Canadian Cancer Society’s Advisory Committee on Cancer Statistics . Canadian cancer statistics 2017. Toronto, ON: Canadian Cancer Society; 2017. Available from: www.cancer.ca/~/media/cancer.ca/CW/cancer%20information/cancer%20101/Can.... Accessed 2017 Nov 15.
-
- Cancer Care Ontario . ColonCancerCheck screening recommendations summary—2016. Toronto, ON: Cancer Care Ontario; 2016. Available from: https://www.cancercareontario.ca/sites/ccocancercare/files/assets/CCCScr.... Accessed 2017 Nov 15.
-
- Provenzale D, Jasperson K, Ahnen DJ, Aslanian H, Bray T, Cannon JA, et al. Colorectal cancer screening, version 1.2015. J Natl Compr Canc Netw. 2015;13(8):959–68. - PubMed
-
- Robertson DJ, Lee JK, Boland CR, Dominitz JA, Giardiello FM, Johnson DA, et al. Recommendations on fecal immunochemical testing to screen for colorectal neoplasia: a consensus statement by the US Multi-Society Task Force on Colorectal Cancer. Am J Gastroenterol. 2017;112(1):37–53. Epub 2016 Oct 18. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials