Global and Regional Ventilation during High Flow Nasal Cannula in Patients with Hypoxia
- PMID: 31723854
- PMCID: PMC6849003
- DOI: 10.4266/acc.2017.00507
Global and Regional Ventilation during High Flow Nasal Cannula in Patients with Hypoxia
Erratum in
-
Erratum to "Global and regional ventilation during high flow nasal cannula in patients with hypoxia".Acute Crit Care. 2021 May;36(2):173. doi: 10.4266/acc.2017.00507.e1. Epub 2021 May 28. Acute Crit Care. 2021. PMID: 34078031 Free PMC article. No abstract available.
Abstract
Background: High flow nasal cannula (HFNC) is known to increase global ventilation volume in healthy subjects. We sought to investigate the effect of HFNC on global and regional ventilation patterns in patients with hypoxia.
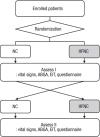
Methods: Patients were randomized to receive one of two oxygen therapies in sequence: nasal cannula (NC) followed by HFNC or HFNC followed by NC. Global and regional ventilation was assessed using electric impedance tomography.
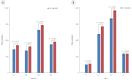
Results: Twenty-four patients participated. Global tidal variation (TV) in the lung was higher during HFNC (NC, 2,241 ± 1,381 arbitrary units (AU); HFNC, 2,543 ± 1,534 AU; P < 0.001). Regional TVs for four iso-gravitational quadrants of the lung were also all higher during HFNC than NC. The coefficient of variation for the four quadrants of the lung was 0.90 ± 0.61 during NC and 0.77 ± 0.48 during HFNC (P = 0.035). Within the four gravitational layers of the lung, regional TVs were higher in the two middle layers during HFNC when compared to NC. Regional TV values in the most ventral and dorsal layers of the lung were not higher during HFNC compared with NC. The coefficient of variation for the four gravitational layers of the lung were 1.00 ± 0.57 during NC and 0.97 ± 0.42 during HFNC (P = 0.574).
Conclusions: In patients with hypoxia, ventilation of iso-gravitational regions of the lung during HFNC was higher and more homogenized compared with NC. However, ventilation of gravitational layers increased only in the middle layers. (Clinical trials registration number: NCT02943863).
Keywords: electric impedance; oxygen inhalation therapy; pulmonary ventilation.
Copyright © 2018 The Korean Society of Critical Care Medicine.
Conflict of interest statement
Dräger Korea (Seoul, Korea) provided electric impedance tomography monitor (PulmoVista 500) with data analysis software. The funder had no role in the design, collection, analysis or interpretation of this study. No other potential conflict of interest relevant to this article was reported.
Figures

References
-
- Slutsky AS, Ranieri VM. Ventilator-induced lung injury. N Engl J Med. 2014;370:980. - PubMed
-
- Manley BJ, Dold SK, Davis PG, Roehr CC. High-flow nasal cannulae for respiratory support of preterm infants: a review of the evidence. Neonatology. 2012;102:300–8. - PubMed
-
- Frat JP, Thille AW, Mercat A, Girault C, Ragot S, Perbet S, et al. High-flow oxygen through nasal cannula in acute hypoxemic respiratory failure. N Engl J Med. 2015;372:2185–96. - PubMed
-
- Spoletini G, Alotaibi M, Blasi F, Hill NS. Heated humidified high-flow nasal oxygen in adults: mechanisms of action and clinical implications. Chest. 2015;148:253–61. - PubMed
Associated data
LinkOut - more resources
Full Text Sources
Medical

