Microbial changes in relation to oral mucositis in autologous hematopoietic stem cell transplantation recipients
- PMID: 31729407
- PMCID: PMC6858439
- DOI: 10.1038/s41598-019-53073-w
Microbial changes in relation to oral mucositis in autologous hematopoietic stem cell transplantation recipients
Abstract
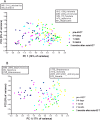
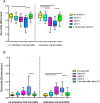
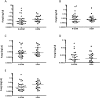
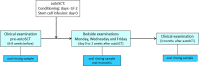
The aim of this prospective, two center study was to investigate the dynamics of the microbial changes in relation to the development of ulcerative oral mucositis in autologous SCT (autoSCT) recipients. Fifty-one patients were diagnosed with multiple myeloma and treated with high-dose melphalan followed by autoSCT. They were evaluated before, three times weekly during hospitalization, and three months after autoSCT. At each time point an oral rinse was collected and the presence or absence of ulcerative oral mucositis (UOM) was scored (WHO scale). Oral microbiome was determined by using 16S rRNA amplicon sequencing and fungal load by qPCR. Twenty patients (39%) developed UOM. The oral microbiome changed significantly after autoSCT and returned to pre-autoSCT composition after three months. However, changes in microbial diversity and similarity were more pronounced and rapid in patients who developed UOM compared to patients who did not. Already before autoSCT, different taxa discriminated between the 2 groups, suggesting microbially-driven risk factors. Samples with high fungal load (>0.1%) had a significantly different microbial profile from samples without fungi. In conclusion, autoSCT induced significant and reversible changes in the oral microbiome, while patients who did not develop ulcerative oral mucositis had a more resilient microbial ecosystem.
Conflict of interest statement
The authors declare no competing interests.
Figures


References
-
- Laheij AM, et al. Oral bacteria and yeasts in relationship to oral ulcerations in hematopoietic stem cell transplant recipients. Supportive care in cancer: official journal of the Multinational Association of Supportive Care in Cancer. 2012;20:3231–3240. doi: 10.1007/s00520-012-1463-2. - DOI - PMC - PubMed
-
- McCann S, et al. The Prospective Oral Mucositis Audit: relationship of severe oral mucositis with clinical and medical resource use outcomes in patients receiving high-dose melphalan or BEAM-conditioning chemotherapy and autologous SCT. Bone marrow transplantation. 2009;43:141–147. doi: 10.1038/bmt.2008.299. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

