Trends in Peritoneal Dialysis Use in the United States after Medicare Payment Reform
- PMID: 31753816
- PMCID: PMC6895485
- DOI: 10.2215/CJN.05910519
Trends in Peritoneal Dialysis Use in the United States after Medicare Payment Reform
Abstract
Background and objectives: Peritoneal dialysis (PD) for ESKD is associated with similar mortality, higher quality of life, and lower costs compared with hemodialysis (HD), but has historically been underused. We assessed the effect of the 2011 Medicare prospective payment system (PPS) for dialysis on PD initiation, modality switches, and stable PD use.
Design, setting, participants, & measurements: Using US Renal Data System and Medicare data, we identified all United States patients with ESKD initiating dialysis before (2006-2010) and after (2011-2013) PPS implementation, and observed their modality for up to 2 years after dialysis initiation. Using logistic regression models, we examined the associations between PPS and early PD experience (any PD 1-90 days after initiation), late PD use (any PD 91-730 days after initiation), and modality switches (PD-to-HD or HD-to-PD 91-730 days after initiation). We adjusted for patient, dialysis facility, and regional characteristics.
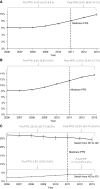
Results: Overall, 619,126 patients with incident ESKD received dialysis at Medicare-certified facilities, 2006-2013. Observed early PD experience increased from 9.4% before PPS to 12.6% after PPS. Observed late PD use increased from 12.1% to 16.1%. In adjusted analyses, PPS was associated with increased early PD experience (odds ratio [OR], 1.51; 95% confidence interval [95% CI], 1.47 to 1.55; P<0.001) and late PD use (OR, 1.47; 95% CI, 1.45 to 1.50; P<0.001). In subgroup analyses, late PD use increased in part due to an increase in HD-to-PD switches among those without early PD experience (OR, 1.59; 95% CI, 1.52 to 1.66; P<0.001) and a decrease in PD-to-HD switches among those with early PD experience (OR, 0.92; 95% CI, 0.87 to 0.98; P=0.004).
Conclusions: More patients started, stayed on, and switched to PD after dialysis payment reform. This occurred without a substantial increase in transfers to HD.
Keywords: end stage kidney disease; peritoneal dialysis; prospective payment system.
Copyright © 2019 by the American Society of Nephrology.
Figures


Comment in
-
Public Policy and Patient Choice of Dialysis Modality.Clin J Am Soc Nephrol. 2019 Dec 6;14(12):1677-1678. doi: 10.2215/CJN.12151019. Epub 2019 Nov 21. Clin J Am Soc Nephrol. 2019. PMID: 31811083 Free PMC article. No abstract available.
References
-
- US Renal Data System : USRDS 2017 Annual Data Report: Atlas of End-Stage Renal Disease in the United States, Bethesda, MD, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, 2017
-
- Wong B, Ravani P, Oliver MJ, Holroyd-Leduc J, Venturato L, Garg AX, Quinn RR: Comparison of patient survival between hemodialysis and peritoneal dialysis among patients eligible for both modalities. Am J Kidney Dis 71: 344–351, 2018 - PubMed
-
- Tong A, Lesmana B, Johnson DW, Wong G, Campbell D, Craig JC: The perspectives of adults living with peritoneal dialysis: Thematic synthesis of qualitative studies. Am J Kidney Dis 61: 873–888, 2013 - PubMed
-
- Walker RC, Hanson CS, Palmer SC, Howard K, Morton RL, Marshall MR, Tong A: Patient and caregiver perspectives on home hemodialysis: A systematic review. Am J Kidney Dis 65: 451–463, 2015 - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

