Synergistic Effects of Human Platelet-Rich Plasma Combined with Adipose-Derived Stem Cells on Healing in a Mouse Pressure Injury Model
- PMID: 31781237
- PMCID: PMC6874957
- DOI: 10.1155/2019/3091619
Synergistic Effects of Human Platelet-Rich Plasma Combined with Adipose-Derived Stem Cells on Healing in a Mouse Pressure Injury Model
Abstract
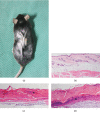
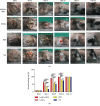
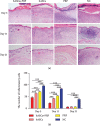
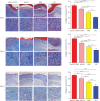
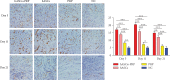
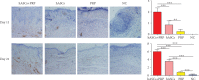
Pressure injury (PI) affects quality of life and results in economic and social burdens. Local transplantation of human adipose-derived stem cells (ASCs) is considered an effective treatment. However, ASC suspension alone is vulnerable to the immune system and results in a shortened cell survival. There is increasing evidence of a synergistic effect of platelet-rich plasma (PRP) combined with ASCs on wound healing. This study investigated the effectiveness, synergy, and mechanism of wound healing following local injection of PRP combined with ASCs in a rodent PI model. PRP or ASCs alone were the control intervention. Wound healing, inflammatory infiltration, collagen deposition, angiogenesis, neurogenesis, and cell homing were investigated. PI healing was promoted by the synergistic effects of PRP combined with ASCs. The combination was more effective than ASCs alone for modulating inflammation, increasing collagen deposition, angiogenesis, neurogenesis, and the persistence of the injected ASCs. These data provide a theoretical foundation for the clinical administration of ASCs combined with PRP in PI healing and skin regeneration.
Copyright © 2019 Zhiyuan Liu et al.
Conflict of interest statement
The authors have no competing financial interests to declare.
Figures


References
-
- Black J., Baharestani M., Cuddigan J., et al. National Pressure Ulcer Advisory Panel’s updated pressure ulcer staging system. Dermatology Nursing. 2007;19(4):343–349. quiz 50. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

