Gentle Manual Acupuncture Could Better Regulate Gastric Motility and Vagal Afferent Nerve Discharge of Rats with Gastric Hypomotility
- PMID: 31781283
- PMCID: PMC6855058
- DOI: 10.1155/2019/9043151
Gentle Manual Acupuncture Could Better Regulate Gastric Motility and Vagal Afferent Nerve Discharge of Rats with Gastric Hypomotility
Abstract
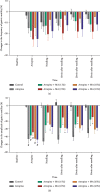
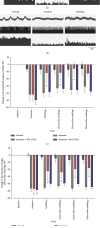
The variation of stimulus intensity of manual acupuncture (MA) may produce diverse acupuncture effects. However, the intensity-effect relationship and the underlying mechanism of MA are still elusive. In this study, the effects of MA regulation of gastric motility were investigated after lifting-thrusting MA treatment with four different frequencies (1 Hz, 2 Hz, 3 Hz, and 4 Hz) at ST36. The experiments were conducted on rats with gastric hypomotility caused by atropine. The results showed that the gastric motility amplitude decreased after atropine injection, while the treatment of four types of MA affected the gastric motility amplitude in varying degrees. Specifically, 2 Hz MA exhibited the most effective results, while 4 Hz MA had the least effect; the effects of 1 Hz MA and 3 Hz MA were between the effects induced with 2 Hz and 4 Hz. Furthermore, the response of gastric vagal afferent nerve discharge and gastric motility was examined after MA treatment with frequencies of 2 Hz and 4 Hz, respectively, on ST36 in order to elucidate the mechanism of MA regulation of gastric motility. The results showed that 2 Hz MA was able to increase the amplitude of gastric motility and discharge frequency of gastric vagal afferent nerves, while 4 Hz MA exhibited seldom effects. These findings suggest that gentle MA (2 Hz) has more stimulating effects than strong stimulation with MA (4 Hz) on gastric hypomotility. In addition, gastric motility regulated by MA was associated with vagal afferent nerve activation.
Copyright © 2019 Yangyang Liu et al.
Conflict of interest statement
The authors declare that there are no conflicts of interest regarding the publication of this paper.
Figures

Similar articles
-
Differential effects of variable frequencies of manual acupuncture at ST36 in rats with atropine-induced inhibition of gastric motility.Acupunct Med. 2016 Feb;34(1):33-9. doi: 10.1136/acupmed-2015-010756. Epub 2015 Jul 15. Acupunct Med. 2016. PMID: 26177688
-
[Characteristics of peripheral afferent nerve discharges evoked by manual acupuncture and electroacupuncture of "Zusanli" (ST 36) in rats].Zhen Ci Yan Jiu. 2008 Feb;33(1):65-70. Zhen Ci Yan Jiu. 2008. PMID: 18386649 Chinese.
-
Strong Manual Acupuncture Manipulation Could Better Inhibit Spike Frequency of the Dorsal Horn Neurons in Rats with Acute Visceral Nociception.Evid Based Complement Alternat Med. 2015;2015:675437. doi: 10.1155/2015/675437. Epub 2015 Jul 15. Evid Based Complement Alternat Med. 2015. PMID: 26257816 Free PMC article.
-
Afferent vagal modulation. Clinical studies of visceral sensory input.Auton Neurosci. 2001 Jul 20;90(1-2):35-40. doi: 10.1016/S1566-0702(01)00265-X. Auton Neurosci. 2001. PMID: 11485290 Review.
-
Manual acupuncture for neuromusculoskeletal disorders: The selection of stimulation parameters and corresponding effects.Front Neurosci. 2023 Jan 30;17:1096339. doi: 10.3389/fnins.2023.1096339. eCollection 2023. Front Neurosci. 2023. PMID: 36793537 Free PMC article. Review.
Cited by
-
Abdominal and Diaphragmatic Mobility in Adults With Chronic Gastritis: A Cross-Sectional Study.J Chiropr Med. 2023 Mar;22(1):11-19. doi: 10.1016/j.jcm.2022.05.004. Epub 2022 Jul 20. J Chiropr Med. 2023. PMID: 36844992 Free PMC article.
-
Influence of acupuncture intensity on analgesic effects in AA rat models.Front Bioeng Biotechnol. 2024 Dec 11;12:1502535. doi: 10.3389/fbioe.2024.1502535. eCollection 2024. Front Bioeng Biotechnol. 2024. PMID: 39723129 Free PMC article.
-
A robot arm-assisted acupuncture system with motion and force monitoring: establishment and validation.Front Bioeng Biotechnol. 2025 Aug 6;13:1563263. doi: 10.3389/fbioe.2025.1563263. eCollection 2025. Front Bioeng Biotechnol. 2025. PMID: 40843449 Free PMC article.
-
The Autonomic Nervous System in Acupuncture for Gastrointestinal Dysmotility: From Anatomical Insights to Clinical Medicine.Int J Med Sci. 2025 May 20;22(11):2620-2636. doi: 10.7150/ijms.107643. eCollection 2025. Int J Med Sci. 2025. PMID: 40520904 Free PMC article. Review.
-
Strong Twirling-Rotating Manual Acupuncture with 4 r/s Is Superior to 2 r/s in Relieving Pain by Activating C-Fibers in Rat Models of CFA-Induced Pain.Evid Based Complement Alternat Med. 2021 Oct 12;2021:5528780. doi: 10.1155/2021/5528780. eCollection 2021. Evid Based Complement Alternat Med. 2021. PMID: 34675986 Free PMC article.
References
-
- World Health Organization. WHO Traditional Medicine Strategy: 2014–2023. Geneva, Switzerland: World Health Organization; 2013. p. p. 76.
-
- World Health Organization. Acupuncture: Review and Analysis of Reports on Controlled Clinical Trials. Geneva, Switzerland: World Health Organization; 2002.
LinkOut - more resources
Full Text Sources

