The Effect of Shear Force on Skin Viability in Patients with Type 2 Diabetes
- PMID: 31781661
- PMCID: PMC6875394
- DOI: 10.1155/2019/1973704
The Effect of Shear Force on Skin Viability in Patients with Type 2 Diabetes
Abstract
Background: Shear is a major risk factor in the development of diabetic foot ulcers, but its effect on the skin of patients with type 2 diabetes mellitus (DM) remains to be elucidated. The aim was to determine skin responses to shear in DM patients with and without diabetic polyneuropathy (DNP).
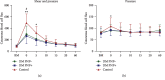
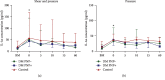
Methods: The forearm skin was loaded with 14.5 N shear (+2.4 kPa pressure) and with 3.5 kPa pressure for 30 minutes in 10 type 2 DM patients without DNP, 10 type 2 DM patients with DNP, and 10 healthy participants. A Sebutape collected IL-1α (measure of tissue damage). A laser Doppler flowmeter measured cutaneous blood cell flux (CBF) as a measure of the reactive hyperaemic skin response.
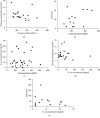
Findings: Reactive hyperaemia and IL-1α release was significantly increased after shear loading in all three groups and was higher compared to the responses to pressure loading. The reactive hyperaemic response after shear loading was impaired in patients with type 2 DM compared to healthy participants but did not differ between patients with and without DNP. The reactive hyperaemic response was negatively correlated with the blood glucose level but did not correlate with the DNP severity score.
Interpretation: Shear is important in the development of tissue damage, but the reparative responses to shear are impaired in patients with type 2 DM. DNP was not associated with altered skin responses, suggesting that the loss of protective sensation to sense shear to skin remains a key factor in the development of diabetic foot ulcers in patients with DNP.
Copyright © 2019 Luuk A. de Wert et al.
Conflict of interest statement
The authors have no conflict of interest and nothing to disclose.
Figures

Similar articles
-
A new method to evaluate the effects of shear on the skin.Wound Repair Regen. 2015 Nov-Dec;23(6):885-90. doi: 10.1111/wrr.12368. Epub 2015 Nov 4. Wound Repair Regen. 2015. PMID: 26426393
-
In diabetic Charcot neuroarthropathy impaired microvascular function is related to long lasting metabolic control and low grade inflammatory process.Microvasc Res. 2015 Sep;101:143-7. doi: 10.1016/j.mvr.2015.07.008. Epub 2015 Aug 1. Microvasc Res. 2015. PMID: 26239695
-
Differences in skin blood flow oscillations between the plantar and dorsal foot in people with diabetes mellitus and peripheral neuropathy.Microvasc Res. 2019 Mar;122:45-51. doi: 10.1016/j.mvr.2018.11.002. Epub 2018 Nov 9. Microvasc Res. 2019. PMID: 30414870
-
Microvascular dysfunction in the context of diabetic neuropathy.Curr Diab Rep. 2014;14(11):541. doi: 10.1007/s11892-014-0541-x. Curr Diab Rep. 2014. PMID: 25189434 Review.
-
Remote ischaemic conditioning in the context of type 2 diabetes and neuropathy: the case for repeat application as a novel therapy for lower extremity ulceration.Cardiovasc Diabetol. 2016 Sep 9;15(1):130. doi: 10.1186/s12933-016-0444-z. Cardiovasc Diabetol. 2016. PMID: 27613524 Free PMC article. Review.
Cited by
-
Tibial cortex transverse transport potentiates diabetic wound healing via activation of SDF-1/CXCR4 signaling.PeerJ. 2023 Sep 15;11:e15894. doi: 10.7717/peerj.15894. eCollection 2023. PeerJ. 2023. PMID: 37727693 Free PMC article.
-
Diabetic foot: Which one comes first, the ulcer or the contracture?World J Orthop. 2021 Feb 18;12(2):61-68. doi: 10.5312/wjo.v12.i2.61. eCollection 2021 Feb 18. World J Orthop. 2021. PMID: 33614425 Free PMC article. Review.
-
Biophysical and biochemical changes in skin health of healthcare professionals using respirators during COVID-19 pandemic.Skin Res Technol. 2023 Jan;29(1):e13239. doi: 10.1111/srt.13239. Epub 2022 Nov 16. Skin Res Technol. 2023. PMID: 36382670 Free PMC article.
-
Impact of shear stress on sacral pressure injury from table rotation during laparoscopic colorectal surgery performed in the lithotomy position.Sci Rep. 2024 Apr 28;14(1):9748. doi: 10.1038/s41598-024-60424-9. Sci Rep. 2024. PMID: 38679609 Free PMC article.
-
Plantar Kinetics During Wheeled Knee Walker Use Compared to Different Assistive Walking Devices in Persons With Type 2 Diabetes Mellitus.Foot Ankle Orthop. 2024 Mar 19;9(1):24730114241235911. doi: 10.1177/24730114241235911. eCollection 2024 Jan. Foot Ankle Orthop. 2024. PMID: 38510515 Free PMC article.
References
-
- Schaper N. C., van Netten J. J., Apelqvist J., Lipsky B. A., Bakker K., on behalf of the International Working Group on the Diabetic Foot (IWGDF) Prevention and management of foot problems in diabetes: a summary guidance for daily practice 2015, based on the IWGDF guidance documents. Diabetes/Metabolism Research and Reviews. 2016;32:7–15. doi: 10.1002/dmrr.2695. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

